Introduction
Hepatocellular carcinoma (HCC) is the fifth most common tumor and is one of the leading causes of cancer-related death in the world [1,2]. The number of patients who are suffering from HCC is increasing in the United States and western nations [2,3].
Although surgical resection is the treatment of choice for HCC, several minimally invasive therapeutic techniques have been used as alternatives for treatment of HCC. In patients who were diagnosed with multifocal HCCs without vascular invasion or extrahepatic spread and a relatively preserved liver function, transarterial chemoembolization (TACE) is one of the most important curative treatment options [4-6]. TACE using ethiodized oil (Lipiodol, Laboratoire Guerbet, Villepinte, France) mixed with anticancerous agents, has been widely performed. Lipiodol transports the anticancerous drug, and the arterial embolic material helps increase the effect of the anticancerous drug [7]. Lipiodol is radiopaque on fluoroscopy to allow for visualization during the TACE procedure and reveals markedly high attenuation on CT images [8].
After image-guided treatment of HCCs, CT and MRI play a crucial role in assessing the therapeutic efficacy, monitoring local tumor progression during follow-up, and detecting early viable tumor, including residual tumor [9]. Dynamic contrast-enhanced CT findings of HCCs after TACE have been reported widely, and they are familiar to radiologists.
MRI findings of HCCs after TACE have not been widely reported, even though these might reveal variable signal intensity (SI) on T1 and T2-weighted images [8]. Therefore, it is difficult to interpret the SI of HCCs after TACE.
The purpose of this study was to evaluate the MRI findings of non-recurrent nodular HCCs with lipiodol uptake (LHCCs) treated with TACE, focusing especially on SI. Furthermore, we evaluated SI of MRIs for non-recurrent, LHCCs based on the amount of lipiodol and the size of the tumor.
Methods
Our Institutional Review Board (2014-10-007) approved this study and waived acquisition of informed consent due to the retrospective evaluation.
Seventy-two consecutive LHCCs of 68 patients who underwent gadoxetic acid-enhanced MRI at our institution after TACE were retrospectively recruited from April 2009 to June 2014. The time interval between TACE and MRI varied from 17 days to 772 days (average, 224 days). Among them, 28 LHCCs were selected according to the following inclusion and exclusion criteria.
Patients had to have undergone gadoxetic acid-enhanced dynamic MRI after TACE for treatment of HCCs and had a follow-up precontrast CT at least six months after or before undergoing MRI. The time interval between precontrast CT and MRI ranged from 0 to 177 days (average, 17 days). These inclusion criteria were needed to evaluate the SI of MRI compared to the appearance of nodular LHCCs on precontrast CT. If the time interval between the MRI and CT was long, then the amount of lipiodol or the shape of the nodular LHCC could have been altered.
Among the 72 lesions, the following lesions were excluded: 13 LHCCs with marginal recurrence, six HCCs treated with combined radiofrequency ablation (RFA) and TACE, 11 HCCs that were too small size to recognize on MRI, four HCCs with sparse or minimal lipiodol uptake of less than 50%, three infiltrative, non-nodular HCCs, three HCCs with poor quality MRIs, and one HCC with no precontrast CT images after TACE. Ultimately, 28 HCCs from 27 patients showing dense (>90%) and partial (>50%) uptake of lipiodol on precontrast CT images after TACE were enrolled in our study.
MRI examinations were performed with a whole-body 3T MRI unit (Achieva, Philips Medical Systems, Best, The Netherlands). The imaging protocols are as follows. T1-weighted, chemical-shift, gradient-echo, images were initially obtained with a breath-hold, in-phase sequence (TR/TE, 3.50/1.15 msec; flip angle, 10°; field of view, 316×340 mm; matrix, 180×190; slice thickness, 5 mm; slice gap, 5 mm) and an out-of-phase sequence (TR/TE, 3.50/2.30 msec; flip angle, 10°; field of view, 316×340 mm; matrix, 180×190; slice thickness, 5 mm; slice gap, 5 mm). Dynamic acquisition was performed with 3D T1-weighted enhanced high-resolution isotropic volumetric excitation (eTHRIVE), which obtained precontrast, arterial, portal, and equilibrium images at three, ten, fifteen, and twenty minutes after injection of 10 mL gadoxetic acid disodium (Primovist, Bayer Schering Pharma, Leverkusen, Germany) (TR/TE, 3.12/1.50 msec; flip angle, 10°; field of view, 320×340 mm; matrix, 228×226; slice thickness, 4 mm; slice gap, 2 mm). Diffusion-weighted images (DWI) with several b values were obtained (TR/TE, 1,509.80/54.71 msec; b value, 0/50/400/800 sec/mm2; flip angle, 90°; field of view, 340×340 mm; matrix, 112×108; slice thickness, 5 mm; slice gap, 5 mm). T2-weighted images (T2WI) were obtained by single shot high-resolution turbo spin echo (TR/TE, 985.77/80 msec; flip angle, 90°; field of view, 316×340 mm; matrix, 324×271; slice thickness, 5 mm; slice gap, 5 mm).
Two radiologists (one abdominal imaging specialist and one third year resident) retrospectively reviewed all MRI and CT images with consensus.
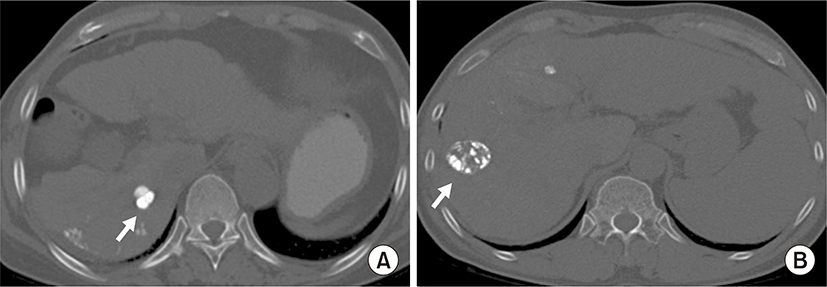
HCCs were analyzed according to the amount of lipiodol uptake on precontrast CT images with bone window setting and were divided into two groups. Group A included 16 HCCs with dense uptake of lipiodol (more than 90%), and group B included 12 HCCs with partial uptake of lipiodol (between 50% and 90%) (Fig. 1). The HCCs which uptook lipiodol less than 50% will be have fewer effect of lipiodol on MR SI, therefore we only included the HCCs showing dense (>90%) and partial (>50%) uptake of lipiodol on precontrast CT images.
For HCC size analysis, we divided the two groups of LHCCs according to the longest diameter of the tumor. Group I was defined by a diameter of less than 2 cm (n=12), and group II was defined by a diameter of greater than or equal to 2 cm (n=16). Tumor size ranged from 0.6 cm to 5.2 cm (average, 2.1 cm). Because the LHCCs of less than 2cm had similar tendency of the MR SI and also group II showed similar, we grouped LHCCs by the 2cm of the tumor diameter.
We retrospectively evaluated SI on the MRIs of LHCCs based on the amount of lipiodol uptake and tumor size. The SI of the HCCs on MRI was classified as high, iso, mixed (high and low), and low when compared to the normal liver parenchyma. We evaluated whether LHCCs were enhanced on dynamic contrast-enhanced MRIs or not.
Results
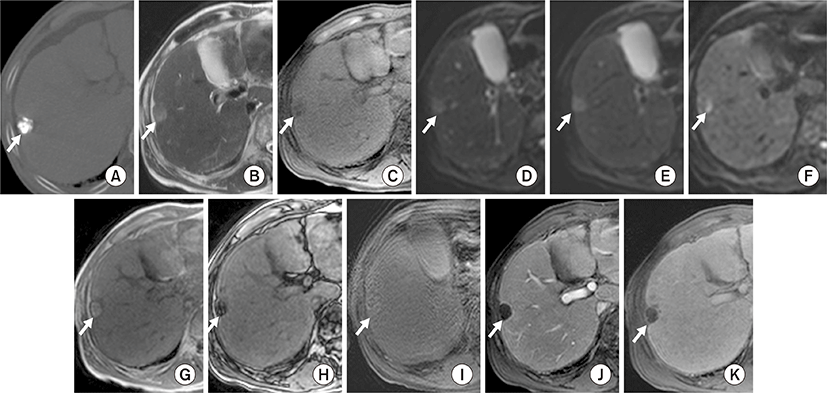
Among the 16 dense LHCCs in group A, eight LHCCs (53%) showed high SI, and five LHCCs (33%) showed iso SI on T2WI. Ten LHCCs (63%) showed low SI, and three LHCCs (19%) showed iso SI on T1WI. At b values of 0, 50 400, and 800, high SI was seen on DWI in seven, eight, eight, and five LHCCs, respectively. Six LHCCs (38%) showed decreased SI when compared to liver parenchyma at higher DWI b values of 400 and 800. Nine LHCCs (56%) showed high SI on in-phase gradient-echo images (GE), and ten LHCCs (63%) showed low SI on out-of-phase GE. None of the 16 LHCCs were enhanced on dynamic contrast-enhanced images (Table 1, Fig. 2).
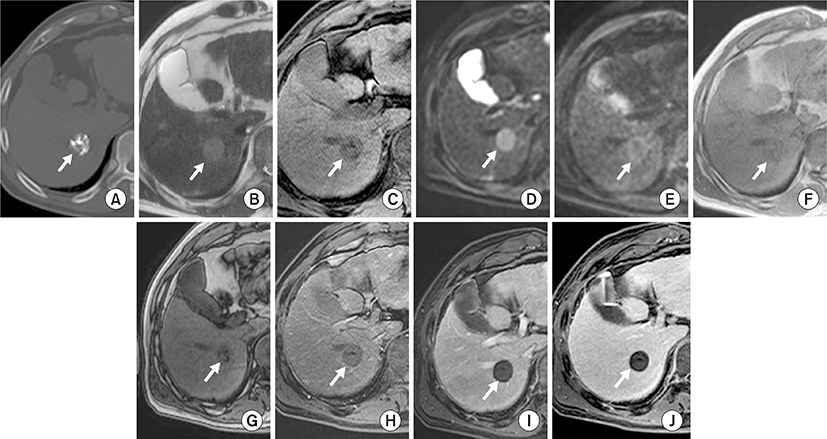
Among the 12 partial LHCCs in group B, six LHCCs (50%) revealed high SI, and four LHCCs (33%) revealed mixed SI on T2WI. Six LHCCs (50%) revealed low SI, and four LHCCs (33%) revealed mixed SI on T1WI. At b values 0, 50, 400, and 800 high SI was observed on DWI in six, seven, seven, and six LHCCs, respectively. Ten LHCCs (83%) revealed decreased SI when compared to liver parenchyma at higher DWI b values of 400 and 800. Six LHCCs (50%) revealed high SI on in-phase GE, and seven LHCCs (58%) revealed low SI on out-of-phase GE. None of the 12 LHCCs were enhanced on dynamic contrast-enhanced images (Table 1, Fig. 3).
According to the size of HCCs, all 12 LHCCs (100%) in group I revealed dense uptake of lipiodol, compared to five of 16 LHCCs (31%) in group II that revealed dense uptake of lipiodol.
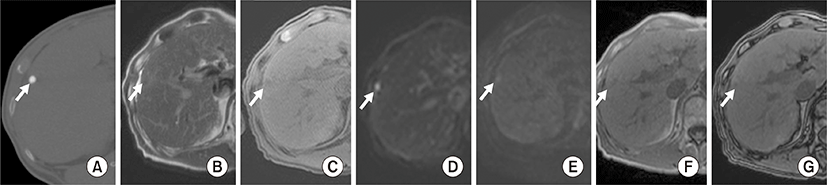
In group I, six LHCCs (50%) showed high SI, and four LHCCs (33%) showed iso SI on T2WI. On T1WI, six LHCCs (50%) showed low SI, and three LHCCs (25%) showed iso SI. At b values of 0, 50, 400, and 800, iso SI was seen on DWI in eight, seven, six, and seven LHCCs, respectively. Six LHCCs (50%) showed decreased SI on DWI at higher b values of 400 and 800) (Table 2, Fig. 4).
In group II, eight LHCCs (53%) revealed high SI, and four LHCCs (27%) revealed mixed SI on T2WI. No LHCCs showed low SI on T2WI; however, low SI was seen on T1WI in ten LHCCs (63%). Four LHCCs (25%) revealed mixed SI on T1W1. At b values of 0, 50, 400, and 800, DWI revealed high SI in nine, ten, ten, and eight LHCCs, respectively. Eleven LHCCs (69%) revealed decreased SI on DWI at higher b values of 400 and 800 (Table 2).
Among the total 28 LHCCs, 14 LHCCs (52%) revealed high SI, and seven LHCCs (26%) revealed iso SI on T2WI. Sixteen LHCCs (57%) revealed low SI, and five LHCCs (18%) revealed mixed SI on T1WI. At b values of 0, 50, 400, and 800 DWI showed high SI in 13, 15, 15 and 11 LHCCs, respectively. Sixteen LHCCs (57%) showed decreased SI at higher b values of 400 and 800. Fifteen LHCCs (54%) showed high SI on in-phase GE, and 17 LHCCs (61%) showed low SI on out-of-phase GE.
Discussion
TACE is commonly performed to treat unresectable HCC and most secondary liver cancers. The purpose of TACE is to destroy the tumor and to deliver chemotherapeutic agents along with iodized oil and embolic material directly to the tumor. As a result, the tumor is exposed to a high concentration of chemotherapeutic agents for a prolonged period of time [10,11]. Therefore, TACE may cause acute ischemic damage to the HCC, and can cause coagulation necrosis, as the hepatic artery is the only artery that nourishes the HCC [12].
Buckwalter et al. [13] reported that ethiodol (ethionized oil), a lipid-soluble iodate contrast medium used in lymphangiography, modified lymph node signaling by reducing T1 and increasing T2 relaxation time. Thus lymph nodes were not distinguished from subcutaneous fatty tissue. Lipiodol is a mixture of ethyl esters from iodurate fatty acids of plant origin and has the same effects on the HCCs in which it accumulates. De Santis et al. [14] reported that pure lipiodol showed a high SI on T1WI (higher than that of subcutaneous fatty tissue) and a low SI on T2WI (lower than that of subcutaneous fatty tissue). Therefore, lipiodol can show increased SI in both T1 and T2WI [14].
De Santis et al. [14] reported that HCCs treated by TACE within one week showed high SI on T1WI, but HCCs treated by TACE after three months revealed variable SI on T1WI. A high concentration of lipiodol immediately after TACE led to high SI; however, this concentration was too low to modify the intensity some period after TACE.
In our study of 28 LHCCs, only four showed high SI, but 16 LHCCs revealed low SI on T1WI. This may be because we obtained T1WIs with a fat suppression technique prior to dynamic contrast-enhanced imaging to detect enhancing lesions. Because lipiodol is a fatty acid, we hypothesized that it caused low SI on fat suppression T1WI.
In our cases of GE images, 15 LHCCs (54%) showed high SI on in-phase GE, and 17 LHCCs (61%) showed low SI on out-of-phase GE. This result suggests that because lipiodol has a fatty component, the fat suppression technique may have caused the LHCCs to have high SI on in-phase GE but low SI on out-of-phase GE.
De Santis et al. [14] reported that on T2WI three months following TACE, 25 of 30 HCCs showed decreased SI with statistical significance. They believed this result was due to coagulation necrosis induced by TACE rather than the effect of lipiodol.
Therefore, HCCs treated with TACE have been known to reveal variable SI on unenhanced T1WI and T2WI due to coagulation necrosis and/or iodized oil [12]. Hypointensity on T2WI corresponds to coagulation necrosis, while hyperintensity represents hemorrhage or residual tumor [15]. It has been reported that moderate hyperintensity on T2WI suggests the presence of viable tumor and that T2WI is highly specific [16]. However, it is sometimes difficult to differentiate a viable tumor from necrotic areas on T1WI and T2WI. We think that the presence of hyperintense areas on T2WI does not always represent viable tumor, especially in cases of LHCCs.
Kubota et al. [15] reported that the SI of MRIs was not markedly affected by lipiodol and was useful for evaluating recurrent or residual viable tumor after TACE. However, high signals on precontrast MRIs were a disadvantage of dynamic MRI. On the contrary, our study showed that 14 LHCCs (52%) revealed high SI on T2WI. We thought that these were influenced by the effect of lipiodol and/or post-therapeutic hemorrhage.
Therefore, HCCs treated with TACE have been known to reveal variable SI on unenhanced T1WI and T2WI because coagulation necrosis, iodized oil and post-therapeutic hemorrhage might influence the SI of LHCCs [17-19].
Diffusion weighted imaging (DWI) is sensitive to the microscopic diffusion of protons from water molecule, and it reveals the microenvironment of water diffusion at a cellular level. DWI measures the apparent diffusion coefficient (ADC) quantitatively. In viable tumors, intact membranes limit the mobility of water molecules, and the ADC is lower, which reflects restriction of diffusion [20]. On the other hand, cellular necrosis increases membrane permeability, allowing for increased motion of water molecules, which results in increased diffusion. After TACE, an increased ADC can be explained by treatment-induced necrosis and cell death [21].
In our study, 16 of 28 LHCCs (57%) showed decreased SI on DWI at high b values of 400 and 800. This suggests that coagulation necrosis and cell death may cause a decrease in SI. This finding could help differentiate viable tumor from treatment-induced necrosis, even though uptake of lipiodol.
This study had several limitations. First, the number of patients and LHCCs was small. We ultimately chose 27 patients with 28 LHCCs. For more coherent results about the SI of LHCC, a study with a greater number of LHCCs will be needed. Second, the time intervals between TACE and MRI and between MRI and CT varied due to the retrospective nature of the study. Third, this study was performed by retrospectively. There might be selection bias of patient groups. A prospective study with a large number of LHCCs in the multicenter is needed for further evaluation.
In conclusion, SI of LHCCs was variable on MRI. However, more than half of the LHCCs showed high SI on T2WI, low SI on T1WI, high SI on in-phase GE, low SI on out-of-phase GE, and decreased SI at higher DWI b values, regardless of the degree of lipiodol uptake or tumor size. No LHCCs were enhanced on dynamic contrast-enhanced MRI. These results can aid in interpreting MRI findings of LHCC and to differentiate them from recurrent HCCs. The radiologist should know these MRI findings to allow for proper interpretation and diagnosis.