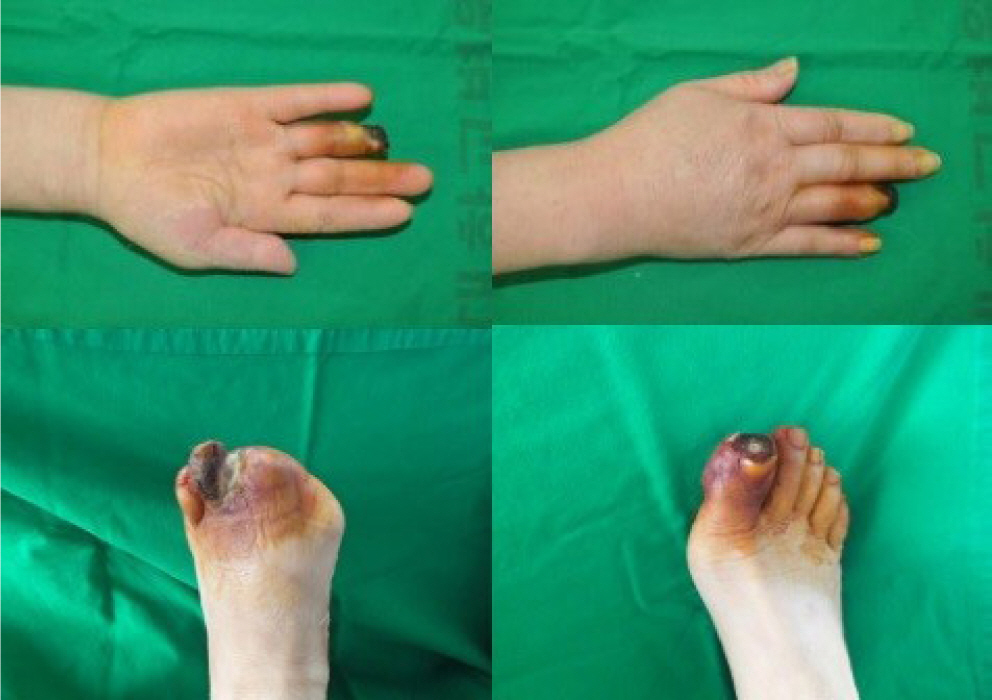
Symmetrical peripheral gangrene is a severe condition marked by symmetric acral necrosis without obstruction of the major blood vessels. This case report examines the critical decisions involved in choosing between early and delayed amputation, as well as determining the extent of the necessary amputation. We present three cases: one involving antiphospholipid syndrome, another with disseminated intravascular coagulation, and a third associated with diabetes mellitus. All three cases ultimately required amputation due to symmetrical peripheral gangrene. In the first two cases, amputation was delayed, which is typically advantageous as it allows for the clear demarcation of necrotic tissue. However, in the third case, where infection was evident, immediate amputation was necessary despite the patient's overall poor health.
 , Seo Hwa Park
, Seo Hwa Park , Eun Gyu Kang
, Eun Gyu Kang , Gyu Cheon Kyung
, Gyu Cheon Kyung , Hyo Dong An
, Hyo Dong An , So-Yeon An
, So-Yeon An
Mucormycosis is a rare disease caused by fungi. Most commonly involved sites of mucormycosis infection are sinuses, lungs, skin and soft tissues. Systemic risk factors for mucormycosis are diabetes mellitus, neutropenia, corticosteroid use, hematological malignancies, organ transplantation, metabolic acidosis, deferoxamine use and advanced age. Local risk factors are history of trauma, burns, surgery and motor vehicle accidents. We present a case of cutaneous mucormycosis in a patient with diabetes mellitus. A 66-year-old female with uncontrolled diabetes mellitus, admitted with necrotizing lesion after minor abrasions on leg. We took a culture of the lesion and it is diagnosed with mucormycosis. Disease progressed despite administration of systemic amphotericin B. We performed above-knee amputation and changed antifungal agents into liposomal amphotericin B. A tissue biopsy showed nonseptate, irregularly wide fungal hyphae with frequent right-angle branching. Our case report suggests that patients with risk factors should be observed carefully.
Citations


