Introduction
Norovirus infection is the most frequent cause of foodborne outbreaks in Korea, with most cases occurring between November and April. Although no studies have quantified the disease burden of norovirus infection in Korea, estimates from the United States Centers for Disease Control and Prevention indicate that norovirus causes 19 to 21 million illnesses, approximately 2.27 million outpatient clinic visits, 109,000 hospitalizations, and 900 deaths annually in the United States [
1]. Norovirus is highly contagious, even at very low infectious doses. Transmission typically occurs via the fecal–oral route; however, the virus can also be transmitted through aerosols generated from the vomitus or diarrhea of infected individuals [
2]. Because vaccines and antiviral treatments for norovirus infection are not currently available, excluding symptomatic individuals or those exposed to norovirus from food handling or caregiving activities is considered an important strategy to minimize public health impacts.
Humans are the only reservoir for human-infecting noroviruses; therefore, viral particles present in the stool or vomitus of infected individuals constitute the primary sources of transmission [
2]. Bivalve molluscan shellfish, such as oysters, are of particular concern in norovirus transmission because they typically inhabit or are harvested from coastal areas that are vulnerable to wastewater contamination and can accumulate the virus through filter-feeding [
1]. Consequently, oysters are a well-established vector in foodborne norovirus infections. A UK study reported that oysters accounted for 16% of foodborne norovirus infections between 1992 and 2000 [
3]. A high prevalence of norovirus gastroenteritis in the community represents an important risk factor for shellfish-associated norovirus transmission. Therefore, efforts to reduce community-level norovirus incidence should accompany measures aimed at controlling shellfish-related norovirus transmission.
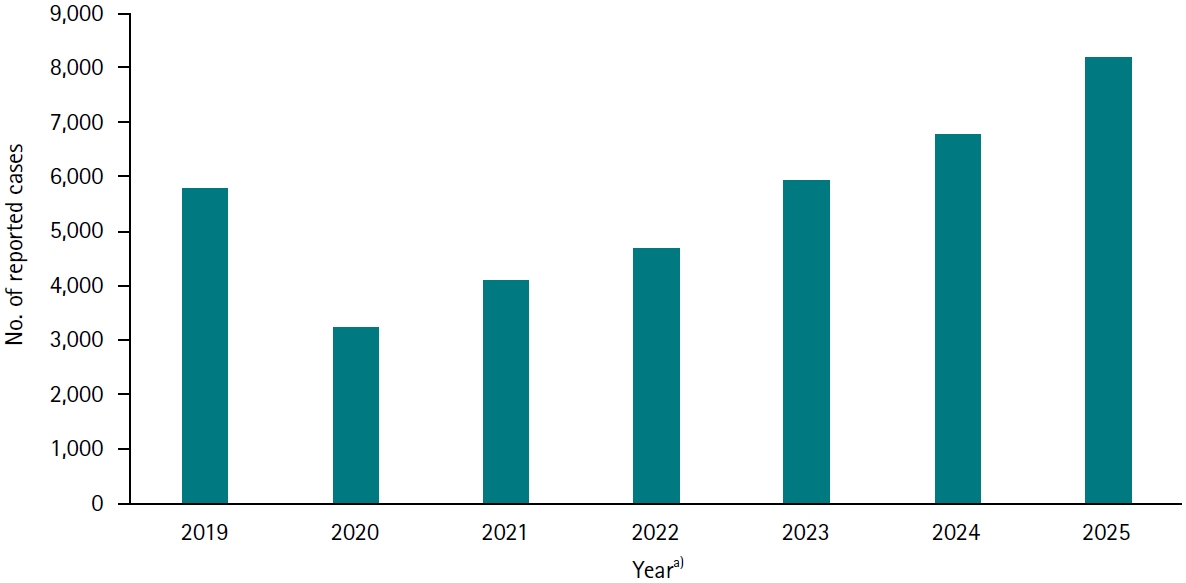
The incidence of norovirus infection in Korea declined in 2020, likely as a result of countermeasures implemented during the COVID-19 (coronavirus disease 2019) pandemic; however, it has increased since 2021. According to the Korean sentinel surveillance system, 3,219 cases of norovirus infection were reported in 2020, a number that doubled to 6,766 in 2024. As of the 46th week of 2025, the cumulative case count for the year had reached 8,172, indicating a continuing upward trend (
Fig. 1). This report presents key points to consider for the control of norovirus infections in Korea.
Sources of norovirus: oysters for cooking
In Korea, when oysters test positive for norovirus at the market or are harvested from production areas that test positive for norovirus, they are supplied to the market as “oysters for cooking (OfC).” Although there is no formal definition of OfC, the Korean Food Code defines “oysters for eating raw (OfR)” as packaged whole-shell, half-shell, or shelled oysters that can be eaten raw by consumers and that are harvested from areas meeting water-quality standards. Accordingly, OfC can be understood as oysters that do not meet the criteria for OfR. OfC contaminated with norovirus may increase the risk of norovirus infection at the community level for 3 reasons.
First, OfC can cause cross-contamination of other ready-to-eat (RTE) foods through hands, utensils, or kitchen facilities. Norovirus present in OfC can be inactivated when oysters are adequately heated during cooking. However, viral particles transferred to other objects during food preparation are likely to survive and infect susceptible individuals. Second, OfC can increase the risk of norovirus infection among workers or food handlers during production, distribution, and preparation. If primary infections occur among exposed individuals, secondary transmission is highly likely, particularly to other workers or back to oysters via handling. Such transmission can occur even when infected workers are asymptomatic. Third, OfC are often consumed raw despite being designated for cooking, thereby bypassing the heating step. Medicinal products, which are subject to stricter regulation than food, are frequently involved in medication errors that can significantly compromise safety. Given the comparatively lower level of regulatory oversight for food, it is reasonable to expect that OfC may frequently lead to norovirus infection when consumed raw.
Statistics on the volume of OfC distributed to the market and consumed raw in Korea are not publicly available. In addition, no prior research has examined the risks associated with OfC in relation to norovirus infections in Korea. Consequently, it is difficult to assess the contribution of OfC to the observed increase in norovirus infections. However, Article 4, paragraph 3 of the Food Sanitation Act in Korea prohibits the sale of products that are potentially or genuinely contaminated with pathogens [
4]. In the United States, the sale and distribution of potentially contaminated oysters are prohibited by the government [
5]. In the United Kingdom and Japan, contaminated oysters must be recalled and cannot be sold [
6,
7]. Although economic and supply-chain considerations may have influenced current regulatory practices, protection of public health should remain the primary guiding principle when managing potentially contaminated shellfish. Accordingly, Korean regulatory decisions that permit the distribution and sale of oysters that are potentially or genuinely contaminated with pathogens such as norovirus are inconsistent with sound public health policy. Proper regulatory management of OfC should therefore be grounded in valid scientific evidence.
Norovirus transmission in catering, nursing, and childcare settings
Restaurants and childcare facilities are well recognized as settings in which foodborne outbreaks, including norovirus infections, occur frequently. In restaurants, if factors contributing to foodborne diseases are not adequately controlled, causative pathogens can be readily transmitted to a large number of visitors within a short period. In childcare facilities, norovirus infection may lead to serious health complications in children, whose immune systems are still developing. Therefore, minimizing the risk of secondary transmission in these settings is particularly important.
First, the exclusion of food handlers who are infected with or exposed to norovirus should be recommended and actively supported. According to a modeling study of norovirus transmission in restaurants, if infected food workers continue to participate in food preparation, preventive measures such as handwashing, glove use, or toilet cleaning are largely ineffective [
8]. Exclusion of ill employees in these settings can be facilitated through ill employee management policies and the provision of paid sick leave. A 2024 Korean study reported that only 10.3% of restaurants in Seoul had ill employee management policies and that 37.5% provided paid sick leave, underscoring the need to implement policies that support this practice [
9].
Second, proper handling of RTE food should be recommended and supported. RTE food refers to food that is edible without additional preparation to ensure food safety. This concept is critical for preventing foodborne diseases, because contaminated RTE food—resulting from bare-hand contact or the use of soiled gloves—is consumed without a pathogen-destroying step. To promote appropriate handling of RTE food, the correct definition of RTE food should be formally adopted in the Korean Food Code (
Table 1), and policies supporting the use of clean utensils or gloves and preventing bare-hand contact should be developed [
9].
Lastly, in childcare and nursing facilities, symptomatic employees and teachers should be immediately excluded from work. Similarly, symptomatic children should not attend school or nursery. Norovirus infection can only be confirmed through laboratory testing, which requires time to yield results. Therefore, exclusion measures to prevent further transmission must be implemented based on clinical symptoms, such as vomiting or diarrhea, rather than being delayed until laboratory confirmation is obtained. Policies supporting home care for symptomatic children, such as childcare services and family care leave, require review and improvement as appropriate. Staff must also be trained in proper methods for cleaning vomitus from norovirus-infected individuals, and adequate cleaning equipment should be readily available.
Norovirus infection statistics: a path toward epidemic control
Appropriate norovirus statistics are essential for tracking epidemic trends and estimating the magnitude of outbreaks. However, data from the Ministry of Food and Drug Safety (MFDS) on foodborne outbreaks do not appear to fully reflect the true trend of norovirus infections. For example, the MFDS reported that the number of norovirus foodborne outbreaks in 2024 decreased by 40% compared with 2023. Given the consistently increasing trend observed since 2021, this reported decrease may not accurately represent the underlying epidemiological pattern of norovirus infections [
10]. Accordingly, diverse and detailed data, including modes of transmission and associated risk factors, need to be collected consistently using standardized methods.
Conclusions
The incidence of norovirus infections has increased rapidly in Korea since 2021, highlighting the urgent need for effective countermeasures to control transmission. OfC that are potentially or genuinely contaminated with norovirus may serve as an unrecognized source of infection in the population. Policies related to OfC should therefore be reviewed and amended to ensure safe consumption. In addition, preventive measures that have demonstrated effectiveness, such as exclusion of ill food employees and proper handling of RTE food, should be actively promoted through the implementation of appropriate supporting policies.
-
Authors’ contribution
Conceptualization: JWL. Methodology/formal analysis/validation: JWL. Project administration: JWL. Writing–original draft: JWL. Writing–review & editing: JWL.
-
Conflict of interest
No potential conflict of interest relevant to this article was reported.
-
Funding
None.
-
Data availability
Not applicable.
-
Acknowledgments
None.
-
Supplementary materials
None.
Fig. 1.Annual number of reported norovirus infections in Korea, 2019–2025. Data from the Korea Disease Control and Prevention Agency’s sentinel surveillance system (
https://dportal.kdca.go.kr/pot/index.do).
a)Data up to the 46th week were used for 2025.
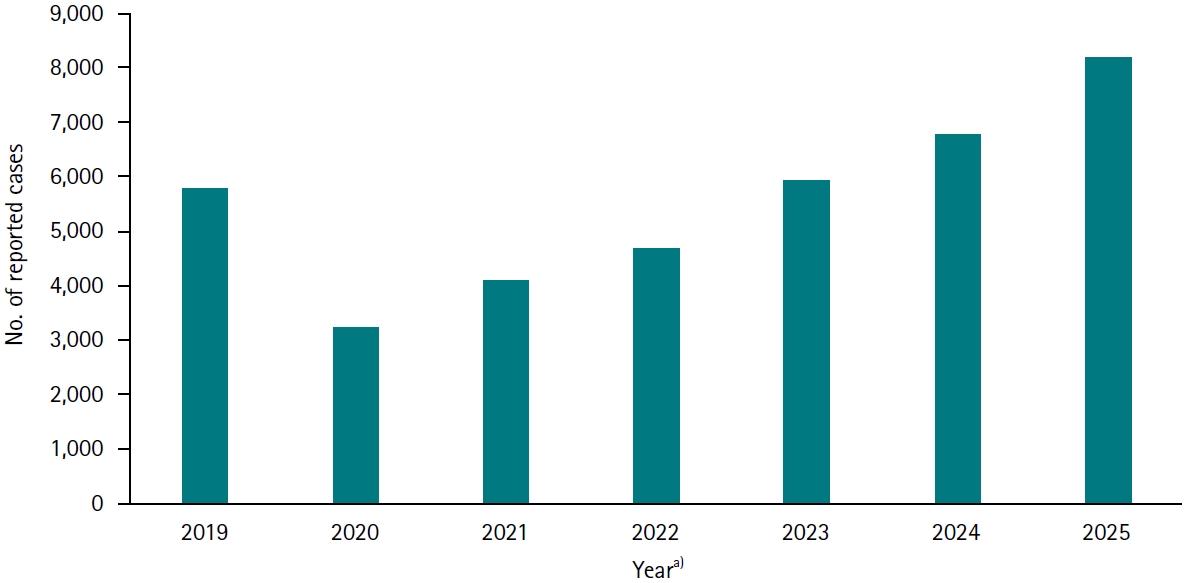
Table 1.Comparison of the definitions of ready-to-eat food
|
Country |
Definition |
|
United States |
“Ready-to-eat food“ is in a form that is edible without additional preparation to achieve food safety |
|
United Kingdom |
A ready-to-eat food is one which is intended to be consumed without any further treatment or processing that would eliminate or reduce pathogens or their toxins to an acceptable level. Examples of ready-to-eat foods include cooked or sliced meats; cheese; washed salads; sandwiches; coleslaw and dips. |
|
Korea |
Ready-to-eat food refers to foods manufactured/processed by adding food or food additives to ingredients of animal/plant origin and intended for direct consumption without further heating or cooking processes; and includes lunch boxes, gimbap (Korean dried seaweed rolls), hamburgers and sunsik (dry grain food), etc. |
References
- 1. U.S. Centers for Disease Control and Prevention (CDC). Centers for Disease Control and Prevention (CDC). Norovirus facts and stats [Internet]. CDC; 2024 [cited 2025 Nov 1]. Available from: https://www.cdc.gov/norovirus/data-research/index.html
- 2. U.S. Centers for Disease Control and Prevention (CDC). CDC Yellow Book 2026: health information for international travel [Internet]. Oxford University Press; 2025 [cited 2025 Nov 1]. Available from: https://www.cdc.gov/yellow-book/hcp/travel-associated-infections-diseases/norovirus.html
- 3. Hassard F, Sharp JH, Taft H, LeVay L, Harris JP, McDonald JE, Tuson K, Wilson J, Jones DL, Malham SK. Critical review on the public health impact of norovirus contamination in shellfish and the environment: a UK perspective. Food Environ Virol 2017;9:123-141. https://doi.org/10.1007/s12560-017-9279-3
- 4. Food Sanitation Act, Law No. 21065 (Oct 1, 2025) [Internet]. Ministry of Government Legislation; 2025 [cited 2025 Nov 1]. Available from: https://www.law.go.kr/법령/식품위생법
- 5. U.S. Food and Drug Administration (FDA). FDA advises restaurants and retailers not to serve or sell and consumers not to eat certain frozen, raw, half-shell oysters from Republic of Korea potentially contaminated with norovirus [Internet]. FDA; 2025 [cited 2025 Nov 1]. Available from: https://www.fda.gov/food/alerts-advisories-safety-information/fda-advises-restaurants-and-retailers-not-serve-or-sell-and-consumers-not-eat-certain-frozen-raw-1
- 6. Food Standards Agency (FSA). Outbreaks of norovirus in raw oysters and their management [Internet]. FSA; 2023 [cited 2025 Nov 2]. Available from: https://www.food.gov.uk/business-guidance/outbreaks-of-norovirus-in-raw-oysters-and-their-management
- 7. Korea Maritime Institute. In Japan, many norovirus food poisoning cases occur due to oyster consumption [Internet]. Korea Maritime Institute; 2025 [cited 2025 Nov 2]. Available from: https://www.kmi.re.kr/globalnews/view.do?rbsIdx=1&key=%EB%85%B8%EB%A1%9C%EB%B0%94%EC%9D%B4%EB%9F%AC%EC%8A%A4&idx=24788
- 8. Duret S, Pouillot R, Fanaselle W, Papafragkou E, Liggans G, Williams L, Van Doren JM. Quantitative risk assessment of norovirus transmission in food establishments: evaluating the impact of intervention strategies and food employee behavior on the risk associated with norovirus in foods. Risk Anal 2017;37:2080-2106. https://doi.org/10.1111/risa.12758
- 9. Lee J, Huh S. Assessing risk factors for foodborne illness in restaurants in Seoul. One Health 2025;20:101009. https://doi.org/10.1016/j.onehlt.2025.101009
- 10. Ministry of Food and Drug Safety (MFDS). The announcement of the food poisoning statistics of 2024, the main cause is salmonella [Internet]. MFDS; 2025 [cited 2025 Nov 2]. Available from: https://www.mfds.go.kr/brd/m_99/view.do?seq=49295
Citations
Citations to this article as recorded by