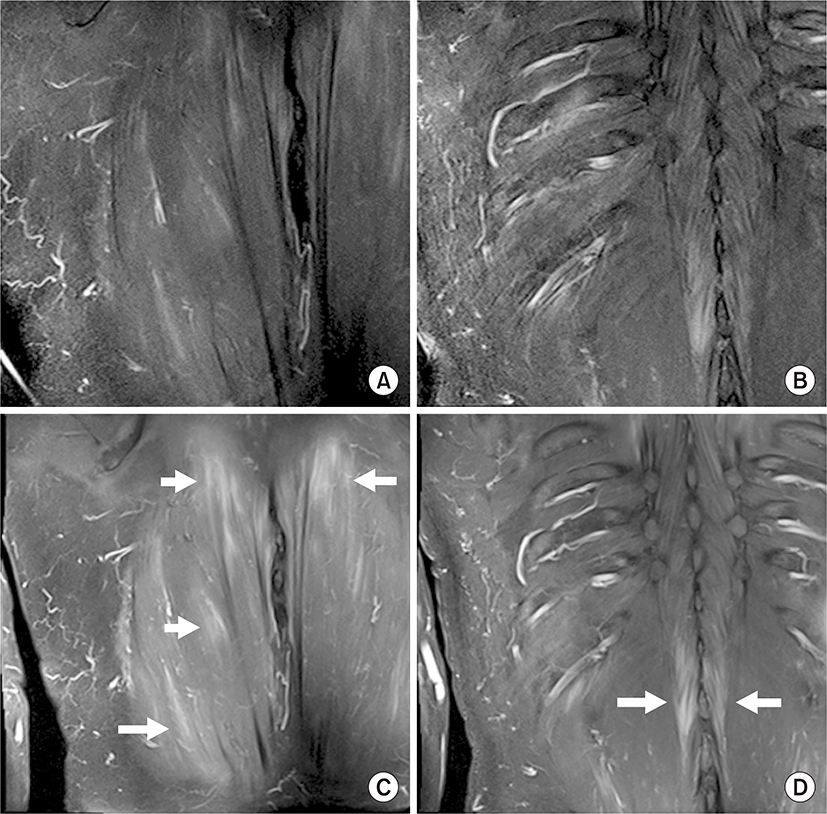
A 58-year-old man had been diagnosed with dermatomyositis and interstitial lung disease in August 2002. Although muscle biopsy was not performed, our patient fulfilled the criteria for dermatomyositis published by Bohan and Peter based on the presence of proximal muscle weakness, elevated serum muscle enzyme levels, electromyographic abnormalities, and dermatomyositis-specific skin alterations [1]. The presence of anti-PL-7 (anti-threonyl-tRNA synthetase) autoantibodies was confirmed by immunoprecipitation after the initial diagnosis. Although he remained in a stable condition while receiving 5 mg prednisolone (PSL) and 150 mg cyclosporine A daily for two years, the patient developed sudden onset of back pain and found a subcutaneous mass on his right upper back. He did not have trauma history and myositis ossificans was not suspected. The subcutaneous mass was approximately 50×50 mm, and mobility was maintained. The subcutaneous tumor surface was smooth, and color change was not observed. Skin rash, proximal muscle weakness, and interstitial lung disease exacerbation were not observed. The serum creatine phosphokinase and serum C-reactive protein levels were elevated (1,575 U/L [normal, 45 to 163 U/L] and 0.72 mg/dL [normal <0.14 mg/dL], respectively). Fat-saturated, T2-weighted magnetic resonance images showed high signal intensity in the bilateral erector spinae muscles (Fig. 1A, B) and strong contrast enhancement was detected by gadolinium-enhanced T1-weighted images (Fig. 1C, D). Tests for procalcitonin and β-D-glucan were negative. Increasing the PSL dose to 30 mg provided complete resolution of clinical symptoms in a few days, including the subcutaneous tumor and back pain, and laboratory examination values returned to normal.
Whole-body magnetic resonance imaging analysis in patients with adult inflammatory myopathies was performed, and myositis was not found in the erector spinae muscles in 63 patients with adult inflammatory myopathies, suggesting that involvement of the erector spinae muscles is a rare complication of adult inflammatory myopathies [2]. Primary erector spinae pyomyositis cases were reported, and abscess was unilateral and localized [3,4]. In the present case, erector spinae muscle myositis was demonstrated to be bilateral, and infectious disease was unlikely to be the cause of erector spinae myositis. Increasing steroid doses in increments completely alleviated his clinical symptoms, including the subcutaneous tumor and back pain, and no relapse occurred after steroid dose reduction. Although skin biopsy was not performed, malignancy was excluded because of good response to steroid therapy. We suspected that the disease state was related to autoimmunity rather than malignancy and infectious diseases. We herein describe a case of dermatomyositis complicated with bilateral erector spinae myositis.