Introduction
Halo nevus is characterized by a round to oval shaped depigmented patch surrounding a precedent skin lesion. Involvement of congenital melanocytic nevus at the center of a halo nevus is reported to be a minor aspect and the patient presenting simultaneous vitiligo is extremely rare [1]. Although the etiology concerning both congenital halo nevus and vitiligo further requires more validity, pathological and laboratory evaluation confirming massive infiltration of CD8 T cells with antibodies directed to melanocytes conjecture similar pathogenesis between the two entities [2]. The causal relationship between the halo and vitiligo loads significant relevance in terms of pathogenesis and disease progression. Herein, the authors present a case of congenital melanocytic nevus along with vitiligo presented concurrently in an adjacent and distant manner.
Case
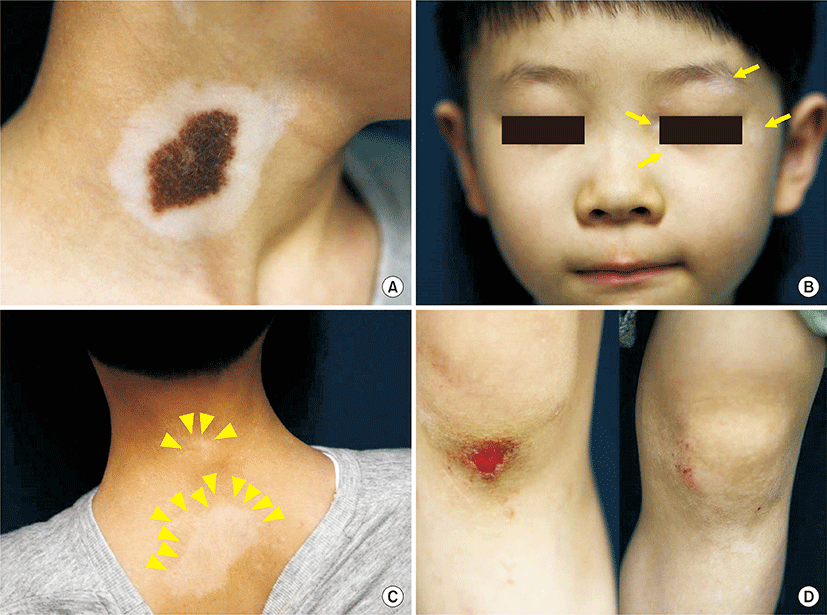
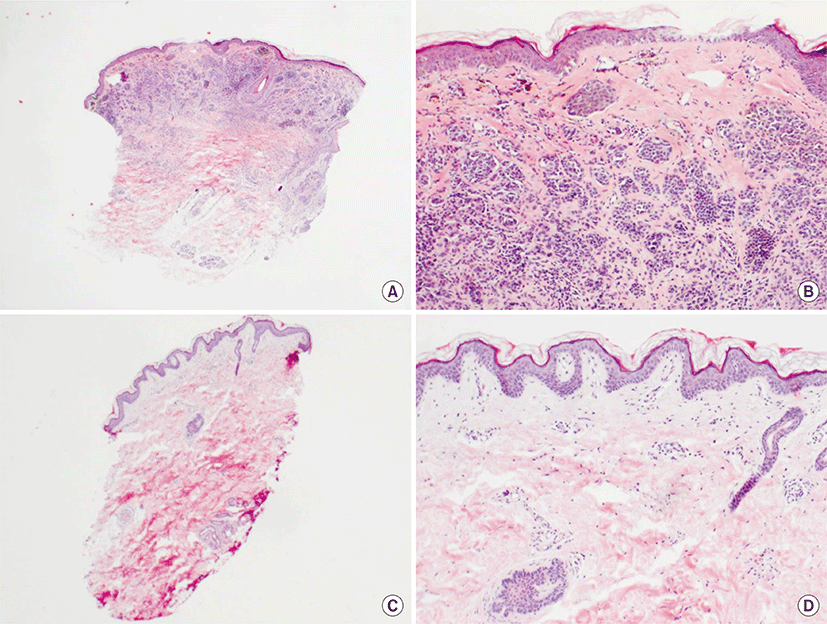
A 6-year-old male presented complaining of recent occurrence of whitish patches on face, both knees and the posterior neck area. A 6 cm-sized hairy and brownish patch surrounded by a whitish patch along the pigmented lesion was noticeable on the neck in addition to the complaint. The patient was born with a congenital melanocytic nevus and the size of the nevus grew in a parallel manner to the height and a depigmented patch surrounding the lesion was developed 3 years in prior to the visit (Fig. 1A). There was no specific family history of skin cancer or significant medical condition. In addition, physical evaluation revealed multiple whitish patches along the face where vision corrective braces were placed and the wound bearing knee area, featuring Koebner phenomenon (Fig. 1B-D). Wood light inspection revealed accentuation at the depigmented. Skin biopsy was performed on the center of the congenital melanocytic nevus and the scanning view revealed heavy infiltration of nevus cells at the upper dermis (Fig. 2A). Middle to lower dermis presented groups of nevus cluster with no definite atypia (Fig. 2B). In addition, skin biopsy was performed on the surrounding whitish area and revealed significant reduction in melanocytes and melanin pigmentation (Fig. 2C). Higher magnification revealed mild infiltration of the lymphocytes (Fig. 2D). Based on the clinical and pathological findings the patient was diagnosed with halo nevus surrounding congenital melanocytic nevus concurrent with vitiligo. The patient was prescribed with tacrolimus 0.03% based ointment and excimer therapy on the whitish patches was delivered.
Discussion
Vitiligo and halo nevus are two common T-cell-mediated autoimmune disorders [3]. Halo nevus is clinically defined as whitish patch surrounding the preceding pigmented lesion and is also known as leukoderma acquisitum centrifugum, Sutton’s nevus, leukopigmentary nevus, perinevoid vitiligo, perinevoid leukoderma [4]. The prevalence of halo nevus was suspected to be 1% in general population and halo nevus accompanied with vitiligo was especially pronounced in children [5]. Moreover, concurrent halo nevus was reported to range from 0.5% to 1.4% in all age groups of vitiligo patients [6]. The majority of the halo nevus arises on acquired nevus followed by congenital melanocytic nevus, melanoma, neurofibroma, seborrheic keratosis and lichen planus. Although, no exact chronological study has been elucidated, halo nevus arising in congenital melanocytic nevus composites 4.7% of all halo nevus and is common under the age of 20 [7]. In addition, the presence of concurrent congenital melanocytic nevus was suspected to be involved with significantly higher occurrence of halo nevus, lower age onset of vitiligo and higher risk for Koebner phenomenon compared to the control group that was without congenital melanocytic nevus [4].
Histologic findings confirm the two diseases as variant type of one another. Barona et al. [8] stated that the presence of a halo nevus indicates a risk factor of vitiligo progression and a prospective observational study suggest that non-segmental vitiligo-associated halo nevus affects age of onset and depigmentation pattern, and has a more frequent familial background of autoimmunity [9]. Moreover, patients with multiple non-segmented vitiligo with congenital melanocytic nevus had a higher frequency of halo nevi at distance, which suggests a relationship between vitiligo and halo nevus [9,10]. This relation was even more significant in halo nevus from congenital melanocytic nevus with higher presentation of vitiligo. Numerous research state that congenital melanocytic nevus can be considered as a possible trigger leading to an earlier development of vitiligo [4].
Although autoimmunity has been suggested to be involved in both diseases, the relationship between vitiligo and halo nevus is not fully understood. CD8+ T lymphocytic infiltration remains as the key role of the disease progression resulting in destruction of melanocytes in both diseases [2,11]. Interferon (IFN)-γ is considered as the key regulative cytokine and induction of IFN-γ leads to up-regulation of chemokine receptors known as CCR5 and CXCR3 [12]. Oxidative stress has also been demonstrated to be enhanced in pathological melanocytes and closely related to melanocyte apoptosis and autoimmune destruction. Oxidative stress triggered by H2O2 accelerates chemokine productions for the recruitment of cytotoxic T cells in lesions of the diseases [3,13]. The clinical similarity presenting both Koebner phenomenons also further states the link.
The presented case features pathologic and clinical similarity of the halo nevus and vitiligo. The immunologic similarity, however, is insufficient as to the order of occurrence differs. Based on the immunologic susceptibility, it has been postulated that the antibodies to congenital melanocytic nevus may precede and affect normal melanocytes to cause lesions consistent that of vitiligo [14]. Microstructural transformation and cellular injury progresses into multiple whitish patches after occurrence of halo nevus. van Geel et al. [4] conjectured improvement in skin lesion after early surgical excision and Workman et al. [15] observed initial improvement after excision of a halo nevus arising in congenital melanocytic nevus. However, elucidation must be supported through sufficient cases and studies. There are currently only three cases reported of halo nevus around congenital melanocytic nevus with concurrent vitiligo in the Korean literature. The present case is to underline the significance of this entity and to alert early management to prevent further complications knowingly, vitiligo.
Informed Consent
Regarding provision of pictorial images, the informed consent was received from parents of the patient in presented Fig. 1B.