Introduction
Minimally invasive surgery for Crohn’s Disease (CD) can be challenging due to thickened and friable mesentery, enteric fistulas, bowel perforation, and frequent occurrence of intra-abdominal abscess. Difficulties in the operative field are reflected by a high rate of conversions and complications following surgical treatment in patients with inflammatory bowel disease [1]. Nevertheless, laparoscopic surgery for patients with intra-abdominal lesions as a result of CD has been widely adopted [2,3]. Moreover, robotic ileocecal resection in patients with CD has been also reported [3–5].
In 2018, Intuitive Surgical launched the da Vinci SP (dVSP) surgical system, which was designed for pure robotic single-incision surgery. It overcame the problem of requiring multiple ports in conventional robotic surgery and addressed concerns involving triangulation and retraction in single-incision laparoscopic surgery. To conduct surgery with a single port, a cannula, which consists of four channels, was applied. Three instruments and one camera can be inserted through a single cannula. Further, the 360° boom can reach anywhere in the abdominal cavity regardless of the surgical target without the need for redocking. For proper triangulation and retraction, each instrument has two joints called the elbow and the wrist joint. In addition, articulating endoscope was adopted to eliminate instrument crashes.
Thus far, there are several reports on the results of minimally invasive approaches, which include laparoscopic and robotic surgery in patients with intra-abdominal CD [3–5]. However, to the best of our knowledge, there has been no report on the application of the dVSP surgical system. Here we report the patient with intra-abdominal CD who underwent simultaneous ileocecectomy and anterior resection due to the fistula between the distal ileum and sigmoid colon.
Case
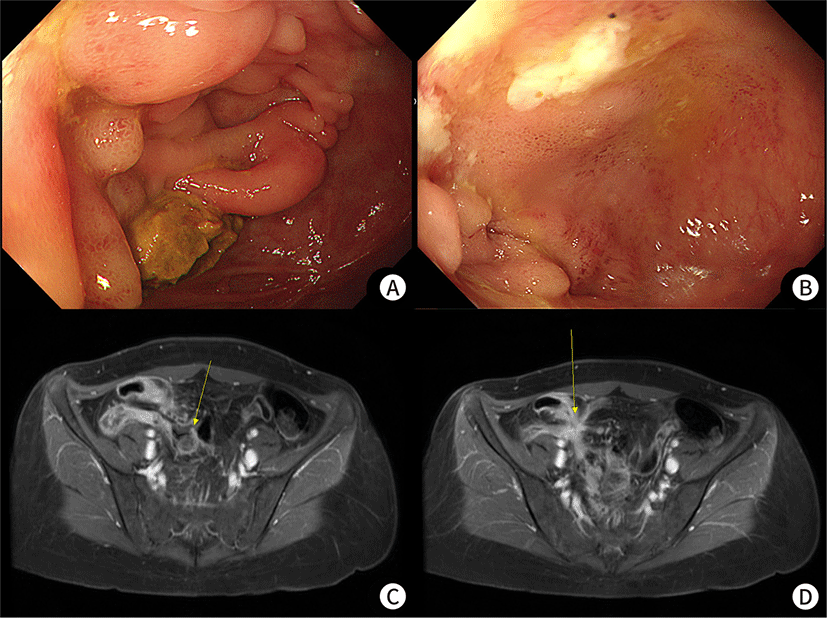
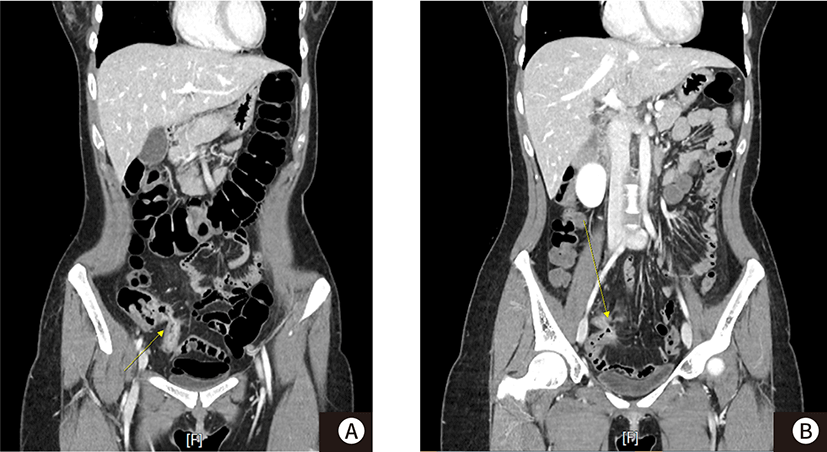
A 25-year-old female visited the clinic with abdominal pain and poor oral intake. She was diagnosed with CD 4 years ago and had been taking infliximab ever since. She had no previous operative history. On admission, her vital signs were non-specific. The blood examination revealed mild elevated leukocyte count (10,010 /mm3; normal, 4.000–10,000 /mm3) and mild elevated C-reactive protein level (3.36 mg/dL; normal, 0–0.5 mg/dL). Colonoscopy showed a whitish scar with inflammatory pseudopolyps in the cecum and a mild structure was observed in the ileocecal valve, although scope passing was possible (Fig. 1A). In the terminal ileum, an ulcer with edematous mucosa and stenosis was observed; here, scope pass was impossible (Fig. 1B). Magnetic resonance enterography demonstrated the progression of a penetrating complication that involved distal ileum with a complex entero-enteric fistula between the terminal ileum and sigmoid colon (Fig. 1C) as well as suspicions regarding another fistula between the distal ileum (Fig. 1D). Despite conservative treatment with bowel rest and antibiotics for 2 weeks, the patient could not tolerate the diet although abdominal pain was relieved. Contrast-enhanced abdominopelvic CT, following conservative treatment, clearly revealed entero-enteric fistula despite improvements in the inflammatory change in the ileum relative to the previous magnetic resonance enterography (Fig. 2). Hence, consultation with the surgical department was conducted.
After careful discussion on surgical treatment with the patient and her family, an operation with the dVSP surgical system was performed. After making a vertical umbilical skin incision of 3.5 cm, the fascia layer was opened using the open Hasson technique. The single-port entry system was applied through the wound opening and CO2 gas to 12 mmHg was insufflated. The patient was placed in the Lloyd-Davies position (i.e., head-down lithotomy with hips flexed) with a steep Trendelenburg position to expose the surgical target (right lower abdomen and pelvis) clearly. The patient cart of the dVSP surgical system was placed on her right side. The dVSP cannula, which consists of four channels, was inserted into the single-port entry system. Three 6-mm robotic instruments (dVSP monopolar curved scissor, fenestrated bipolar forceps, and Cadiere forceps), along with a 12-mm articulating camera, were inserted into each channel. After the completion of docking, the surgeon started to perform robotic surgery in the console. During the console time, the assistant performed endoscopic suction, inserted suture materials into the abdominal cavity, and stapled for distal sigmoid colon resection through the remaining trocar of the single-port entry system.
In the operative field, severe adhesion among terminal ileum, adjacent ileum, and sigmoid colon was observed. To clarify the exact anatomical state, adhesiolysis of the small bowel and right colon was performed. After mobilizing the bowel, the fistula tract between the sigmoid colon and distal ileum was identified and resected. The hole in the sigmoid colon was closed by robotic suture. To perform ileocecectomy, which included lesions of the distal ileum, right colon mobilization to the hepatic flexure was conducted from the right paracolic gutter, duodenum, and Gerota’s fascia. After completing right colon mobilization, sigmoid colon mobilization was performed for the anterior resection, which included the fistula tract. After medial dissection followed by lateral dissection was conducted, the distal sigmoid colon was resected, which included the hole of the fistula tract with a linear stapler intracorporeally administered by an assistant. The proximal sigmoid colon was exteriorized through an umbilical incision and the anvil of the circular stapler was inserted. The bowel was placed back into the abdominal cavity and intracorporeal colo-colic end-to-end anastomosis was performed using a circular stapler (Video clip). Then mobilized right colon and the small bowel were exteriorized through an umbilical incision. Extracorporeal end-to-side anastomosis was performed using a circular and a linear stapler after excision of bowel mesentery with vessel sealer for devascularization. At this point, extensive small bowel exploration was conducted to identify small bowel lesions such as obstruction and stricture due to CD. Although multiple skipped strictures were observed in the ileum and jejunum, strictureplasty is unnecessary because the passage was possible. The operation was over as the drain insertion through the umbilical wound and closure of the main wound was completed (Fig. 3, Supplementary Video 1). Docking, console, and total operation times were 12, 200, and 260 mins, respectively. Estimated blood loss was 50 cc and intraoperative transfusion was not necessary. Ileocecectomy and anterior resection without lymph node dissection were performed simultaneously without any intraoperative events.
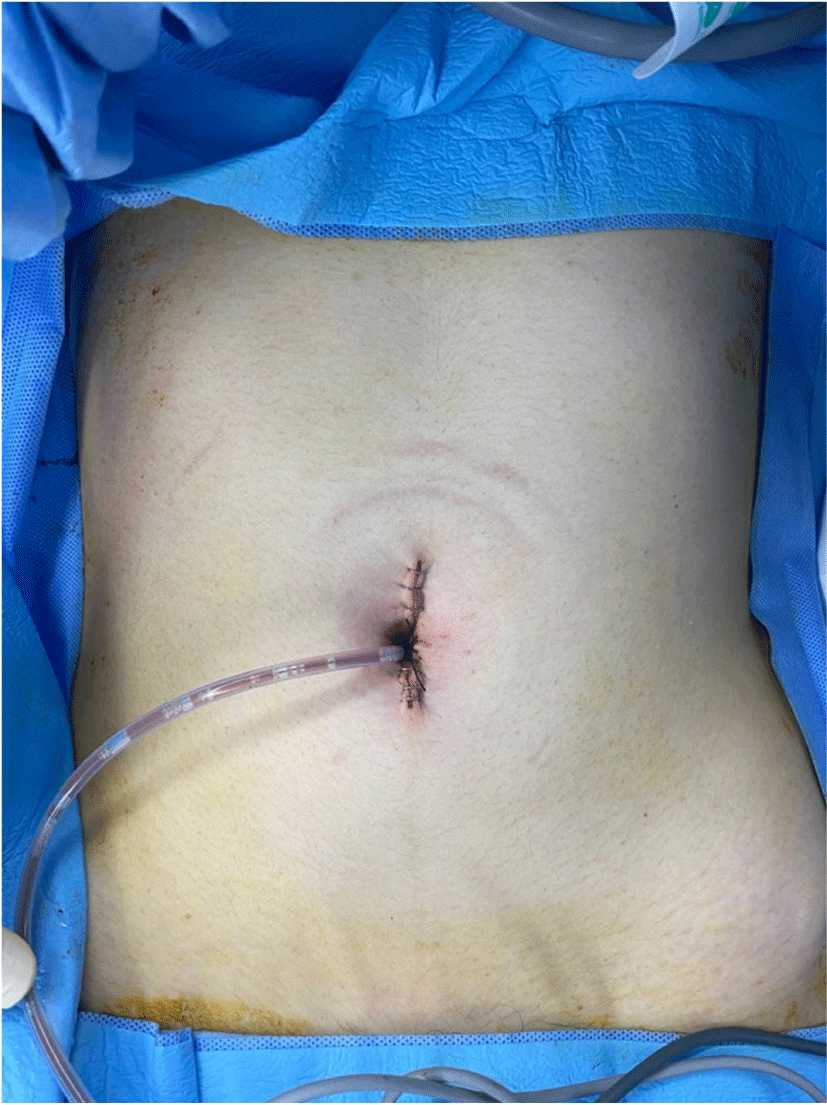
Diet built up in the order of clear liquid, low residue, and regular diet were 1, 2, and 3 postoperative days, respectively. Gas passing and stool passing was detected postoperatively after 4 days. The Foley catheter was removed postoperatively on the first day. Intravenous patient-controlled analgesia and opioids were held on the first postoperative day. The recovery of the patient was uneventful. She was discharged postoperatively on the 8th day. She has been following up with a physician for CD. During the 18-month follow-up period, the CD was well controlled without postoperative complications.
Discussion
Ileocecal resection and primary reconstruction are the most common surgical procedures in patients with CD of the distal ileum and/or the ileo-colon. Surgery in CD can be challenging due to thickened and friable mesentery, enteric fistulas, bowel perforation, and frequent occurrence of intra-abdominal abscesses. However, in selected patients with CD, laparoscopy offers well-described short-term benefits such as decreased pain, lower wound complication rates, earlier resumption of diet and bowel function, better cosmesis, and shorter hospital stay [2,3]. In addition, reduced formation of postoperative adhesions was useful, particularly in young patients who are at significant risk of multiple surgeries [6]. Moreover, Maeda et al. [7] reported the results of single-incision laparoscopic ileocecal resection for CD in their systematic review, suggesting that it may be feasible and safe.
Robotic ileocecal resection has been also attempted in patients with CD. Recently, the results of robotic surgery for CD have been published [3–5]. Hota et al. [3] analyzed and performed a retrospective review of the National Surgical Quality Improvement Program (NSQIP) database to select 5,158 patients with CD who underwent ileocecal resection (open, laparoscopic, or robotic-assisted). In this analysis, the robotic group was composed of 121 patients. Though the robotic-assisted group had significantly longer operative times relative to the laparoscopic surgery group, there was no difference in terms of the postoperative short-term outcomes. Hande Aydinli et al. [4] also reported the safety and feasibility of robotic ileocolic resection for CD compared with laparoscopic approaches. This was accomplished with no leaks, major morbidity/mortality, and comparable length of stay, with a 1-day shorter return of bowel function and lower overall complication rates in 33 robotic patients.
However, previous reports were performed with the two most often used robotic platforms, the da Vinci Si and the da Vinci Xi. There has been no report on robotic surgery with the dVSP surgical system in patients with intra-abdominal CD. We thought that dVSP would have advantages for surgery in patients with CD than previous version of the robotic surgical system. As we use the umbilicus for a single-entry site, all procedures could be performed regardless of the lesion’s location. In particular, it is possible to predict various surgical conditions due to the disease characteristics of CD. Previous versions of robotic systems have limitations in docking multiple devices in this situation. In addition, re-docking is necessary to perform concomitant procedures, such as in our case. As we used the 360° rotation of single-arm devices, we could perform surgery without re-docking for the different workplaces. Many ports and several re-dockings were inevitable if the operation in our case was performed with the previous version of a robotic system or laparoscopic surgery.
Current dVSP model lacks robotic advanced energy instruments and staplers. Advanced energy devices could help simplify the surgery and reduce the operative time. Inflammation can cause bleeding in the mesentery, particularly in patients suffering from CD. In addition, a robot stapler can make intracorporeal anastomosis easier. Gunnells et al. [8] suggested that extensive mesenteric mobilization is not necessary in case the mesentery is intracorporeally divided and an intracorporeal anastomosis is performed. Also, Calini et al. [5] reported that intracorporeal anastomosis was associated with a faster return to bowel function without any impact on the length of stay or 30-day complications compared with extracorporeal anastomosis in patients who underwent robotic ileocecectomy for intra-abdominal CD. The advantages of single-incision robotic surgery can be maximized if robotic advanced energy instruments and staplers are available.
We thought that the dVSP surgery could be performed in patients who can be adapted to other minimally invasive surgical techniques. However, the robotic approach is limited in terms of extensive intracorporeal small bowl explorations due to the docking system, as opposed to the laparoscopic approach, which allows for more freedom of port placement. In particular, dVSP has a hardness in the intracorporeal exploration of the small bowel due to the limitation of movement, relative to previous robotic systems. However, as in our case, if the patient does not have adhesions and has a first-time surgery, an extracorporeal exploration can be performed with the main wound used for trocar insertion.
In conclusion, we successfully performed simultaneous ileocecectomy and anterior resection with the dVSP surgical system for enteric-enteric fistula in a patient with CD. There were no intraoperative events and the patient recovered well without any post-operative complications. To the best of our knowledge, there has been no report on dVSP surgery in patients with intra-abdominal CD. Although more cases are essential for evaluating the feasibility of dVSP surgery in patients with intra-abdominal CD, it can be used in patients who can be adapted to other minimally invasive surgical techniques.

