Introduction
Esophageal subepithelial tumors (SETs) are commonly encountered during screening endoscopy, with an incidence of 0.4% (246/65,233), based on a recent Korean multicenter study [1]. Almost all esophageal SETs are asymptomatic and clinically insignificant, and leiomyomas are the most common. However, malignant SETs, such as gastrointestinal stromal tumors (GISTs) and SET-like carcinomas, can also occur in the esophagus. Endoscopic ultrasonography (EUS) is the most useful diagnostic modality for evaluating SETs of the gastrointestinal tract. The typical EUS features of leiomyomas include well-demarcated, homogeneously hypoechoic lesions with echogenicity similar to that of the surrounding proper muscle layer [2–4]. Calcifications are relatively common in leiomyomas (6.5%–18%); however, cystic changes are rarely observable [5,6]. In contrast, GISTs exhibit typical features on EUS, such as heterogeneously hypoechoic lesions with a marginal halo and hyperechoic spots, and slightly increased echogenicity compared to the surrounding proper muscle layer [5]. Furthermore, irregular margins and cystic changes have been suggested to be predictive factors of malignant potential [7]. Herein, we report a case of symptomatic esophageal leiomyoma with cystic changes on EUS that was managed successfully using thoracoscopic resection.
Case
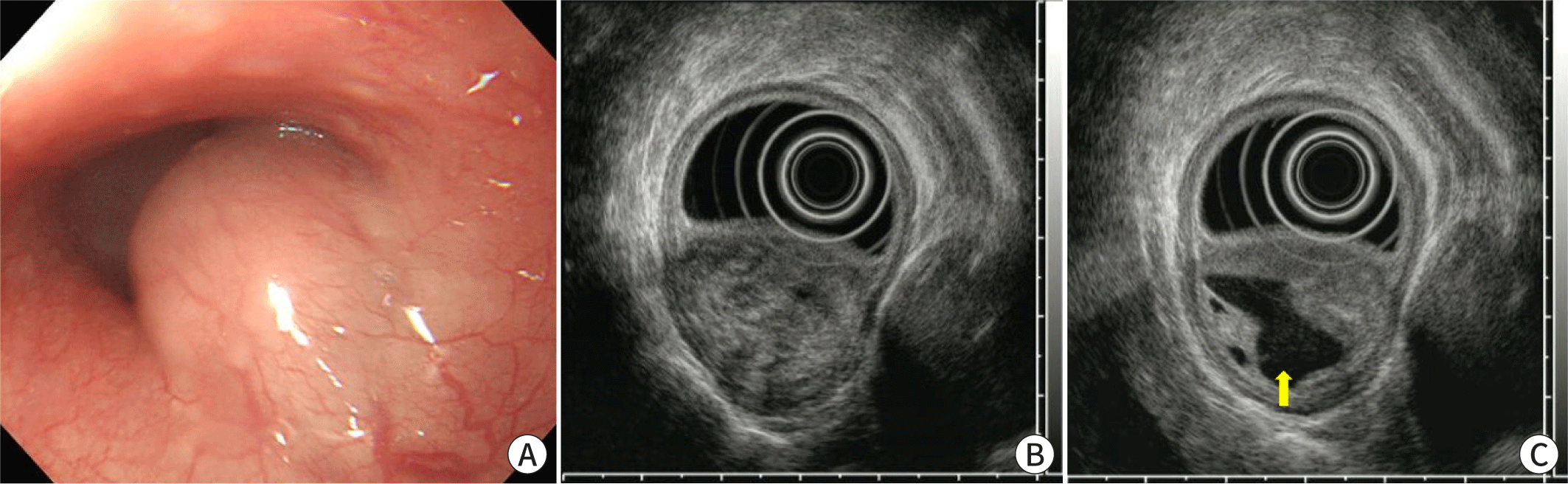
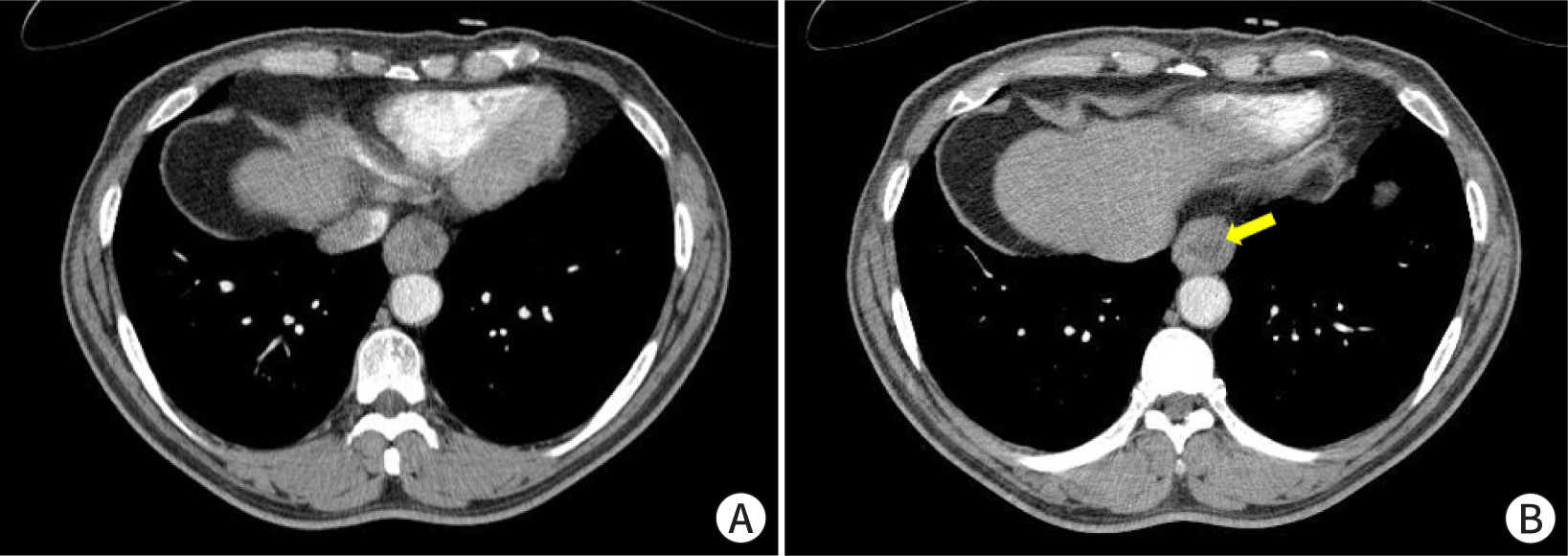
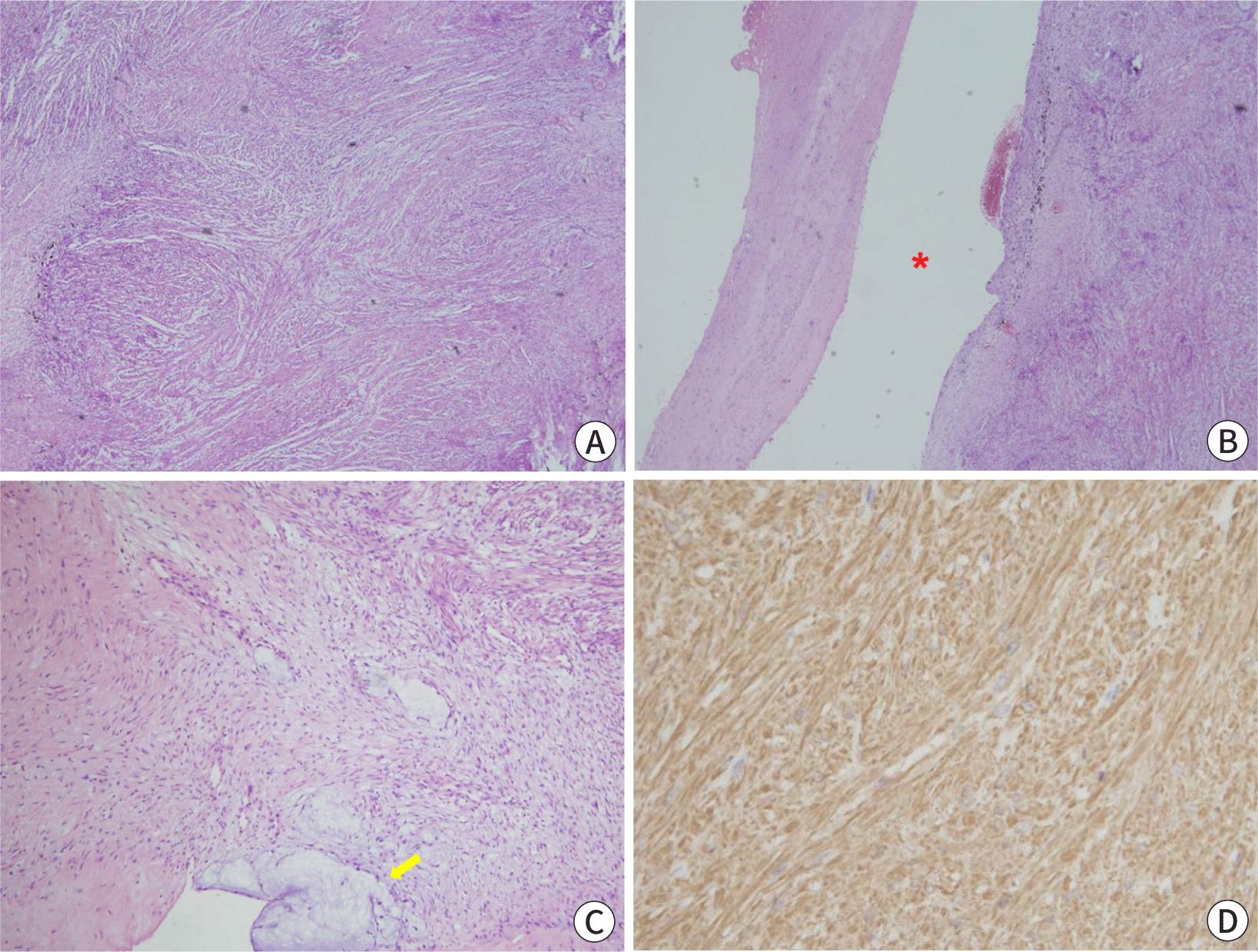
A 65-year-old man presented with an esophageal SET that was incidentally detected during esophagogastroduodenoscopy. The patient had a 1-year history of chest discomfort and dyspepsia, and a 5-year history of diabetes. On endoscopy, the tumor was observed in the lower esophagus and no erosion or ulceration was noted on its surface (Fig. 1A). The tumor was hard and immovable when pressed with biopsy forceps. On EUS, the tumor measured 3.0 cm and had a heterogeneously hypoechoic appearance in the proper muscle layer (Fig. 1B). A cystic change, measuring 1.5 cm, was also noted on the inner side of the tumor (Fig. 1C). These EUS features are suggestive of malignant neoplasms such as GISTs. Physical examination revealed no abnormalities. Laboratory investigations revealed the following: white blood cell count, 5,470 cells/μL; hemoglobin, 15.0 g/dL; platelet count, 193,000 cells/μL; prothrombin time, 10.9 s (international normalized ratio 0.98); aspartate aminotransferase, 32 IU/L; alanine aminotransferase, 45 IU/L; total bilirubin, 0.62 mg/dL; total protein, 7.9 g/dL; albumin, 4.6 g/dL; blood urea nitrogen, 14.3 mg/dL; and creatinine, 0.9 mg/dL. Electrocardiography results were normal. Contrast-enhanced chest CT revealed asymmetric wall thickening with heterogeneous enhancement and a non-enhanced area in the lower esophagus, suggestive of malignant lesions (Fig. 2). Because the patient experienced symptoms, including chest discomfort, and EUS and CT findings were highly suspicious for malignant neoplasms, thoracoscopic resection was performed. Macroscopic examination revealed a well-defined, solid white ovoid mass with cystic changes, measuring 3.2 cm×2.2 cm, in the muscularis propria of the esophagus. Histopathological examination of the specimen revealed intersecting bundles or fascicles of bland spindle cells with eosinophilic cytoplasm (Fig. 3A). Cystic and myxoid degeneration was observed; however, significant cytological atypia, increased mitotic activity, and tumor necrosis were not detected (Fig. 3B, C). Immunohistochemical examination revealed that the tumor cells were positive for smooth muscle actin (Fig. 3D) and desmin, negative for c-kit, CD34, and S-100, and had a low Ki-67 proliferation index (<1%). Accordingly, the tumor was diagnosed as leiomyoma with cystic and myxoid degeneration. The patient’s symptoms, including chest discomfort, subsided completely, and no recurrence was observed at the 24-month follow-up.
Discussion
Esophageal leiomyomas are the most common benign SETs in the esophagus [8]. Unlike GISTs, esophageal leiomyomas do not undergo cystic or myxoid degeneration and are very rarely ulcerated [9]. Almost all patients with esophageal leiomyomas are asymptomatic, but some present with dysphagia, depending on the size of the tumor. In this case, the tumor was not ulcerated, but did exhibit cystic degeneration. This was believed to be the cause of the patient’s symptoms (chest discomfort), which subsided after thoracoscopic resection.
Virtually all esophageal leiomyomas are well-demarcated, homogeneously hypoechoic lesions in the muscularis mucosa or proper muscle layer on EUS, and cystic changes are rarely observed [2,5]. However, in the present case, the esophageal leiomyoma appeared as a well-demarcated but heterogeneously hypoechoic lesion in the proper muscle layer. In addition, the echogenicity of the tumor was greater than that of the surrounding proper muscle layer, and extensive cystic changes were observed. These EUS features are usually highly suggestive of malignant stromal tumors such as GISTs. Chest CT also suggested a malignant rather than a benign lesion. However, EUS and CT cannot perfectly differentiate between benign and malignant SETs. Therefore, EUS-guided fine-needle biopsy has recently emerged as a commonly used diagnostic modality, with an acceptable yield (87.9%) [6,10,11]. In the present case, because the SET was symptomatic and the EUS and CT features were highly suggestive of malignancy, the tumor was surgically resected without histopathological confirmation via EUS-guided fine-needle biopsy.
Histopathologically, both leiomyomas and GISTs are mainly composed of spindle cells and display smooth muscle or nerve sheath differentiation; as such, immunohistochemical analysis is necessary for an accurate diagnosis. Leiomyomas are defined as desmin-positive and c-kit-negative tumors, whereas GISTs are defined as c-kit-positive [12]. The patient described in the present case was ultimately diagnosed with leiomyoma based on immunohistochemical staining.
Because esophageal leiomyomas are benign, resection is not required in most cases. However, when patients experience symptoms, such as dysphagia, the tumor size increases on follow-up examinations or, if the patient strongly desires to undergo tumor resection, resection is needed. In the past, surgical resection, such as thoracoscopic resection, was the primary treatment modality for esophageal leiomyomas located in the muscularis propria. However, endoscopic resection techniques, such as endoscopic submucosal dissection, endoscopic submucosal excavation, and submucosal tunneling endoscopic resection, have recently been introduced and have yielded high complete resection rates [13]. However, when a malignant SET is highly suspected, as in the present case, surgical resection is necessary to achieve satisfactory oncological outcomes.
Esophageal leiomyomas are often encountered as benign lesions during endoscopy. However, these tumors are sometimes symptomatic and do not exhibit the typical EUS and CT features of leiomyomas. In this situation, surgical resection is required to alleviate symptoms and rule out the possibility of malignancy.

