Introduction
During the surgical process suture and tie are most widely used basic techniques in spite of development of automatic stapling device. For optimal wound repair and tissue healing, selection of appropriate suture material for each wound would be trained from the first of the surgical residency. The successful wound healing was achieved by proper suture technique with appropriately selected suture materials. In general, suture materials are classified according to their behavior in tissue (absorbable or non-absorbable), their structure (monofilamanent, or multifilament), and their material (synthetic, organic, or metallic) [1]. A suitable suture does not trigger an inappropriate tissue reaction, but also maintains sufficient tensile strength until proper wound healing is achieved [1].
An ideal suture has the property of being absorbed after complete tissue healing so that a foreign body does not continue to exist in the wound [2]. However, the absorptiveness of suture materials is associated with different advantages and disadvantages leading to a variety of preferences among practicing surgeons. Many surgeons believe that non-absorbable suture materials are superior to absorbable suture materials, because they are easier to tie, are unlikely to break early, and induce a weaker inflammatory response [2]. Others favor absorbable suture materials since they disappear spontaneously and cause less pain and discomfort for the patient [3]. There is still no consensus on which suture material to use, and the choice usually depends on the surgeon’s preference.
In this report, we present a rare case of minute bowel perforation due to a non-absorbable suture material after myomectomy, which may be informative for surgeons regarding the choice of proper suture materials.
Case
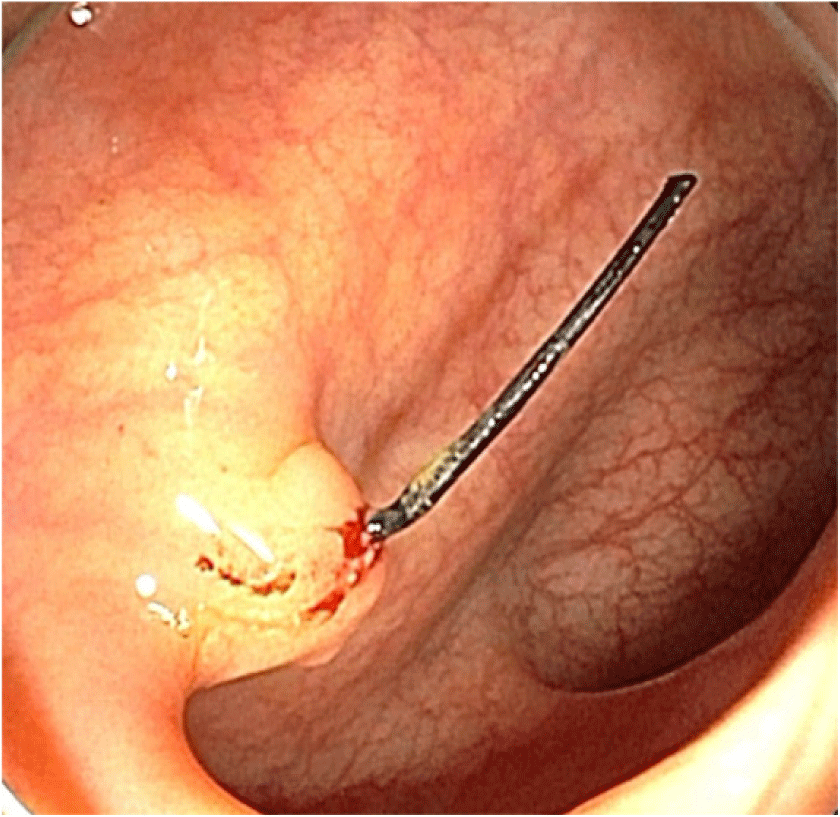
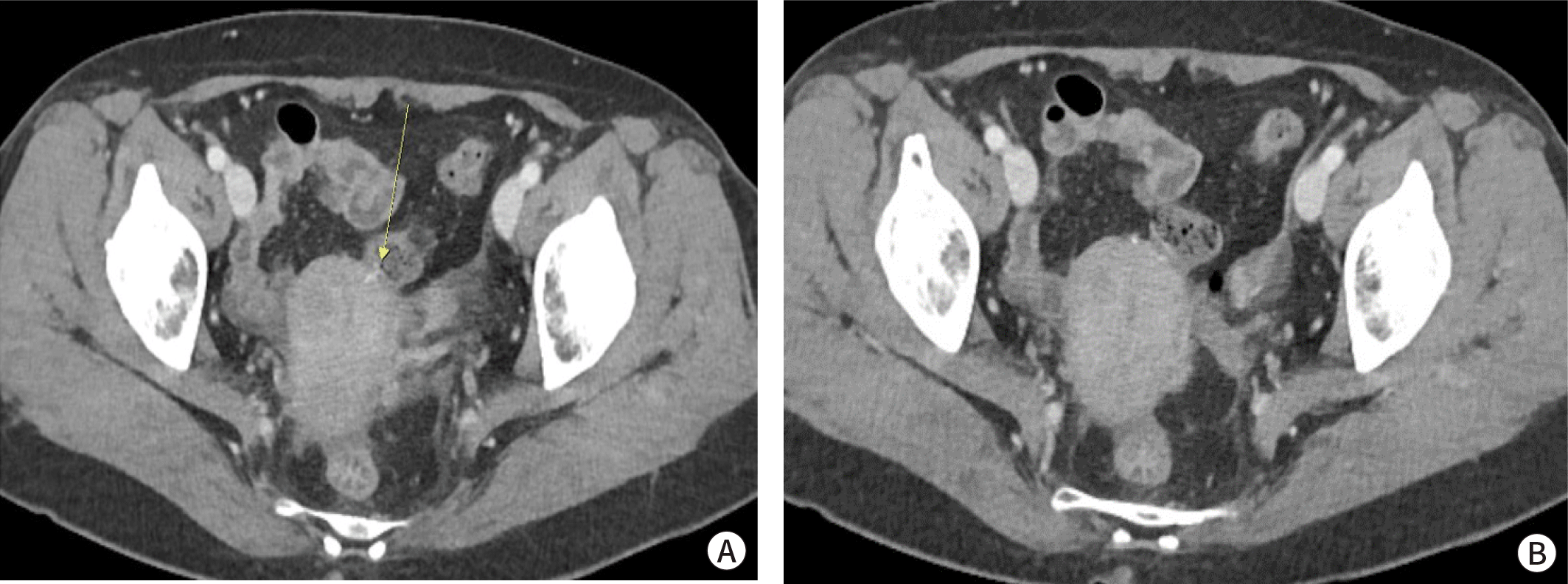
A 60-year-old woman who had no medical disease history except uterine myoma was referred to the colorectal surgery department after colonoscopy. She underwent colonoscopy because of the nonspecific abdominal discomfort lasted for 6 months. Colonoscopy revealed a polypoid lesion with an unknown foreign body at the sigmoid colon (Fig. 1). There was no abnormal findings in previous several routine colonoscopic evaluation. Abdomen-pelvic computed tomography showed radiopaque foreign body that was probably penetrating the uterus and abutting the sigmoid colon (Fig. 2A, 2B). Because of the possibility of colon perforation and previous laparoscopic myomectomy history 15 years ago, we decided to remove the foreign body by laparoscopic approach. The laboratory examinations revealed normal serum levels of white blood cells (3,950/μL; reference range, 4,000-10,000/μL) and C-reactive protein (0.05 mg/dL; reference range, 0-0.5 mg/dL).
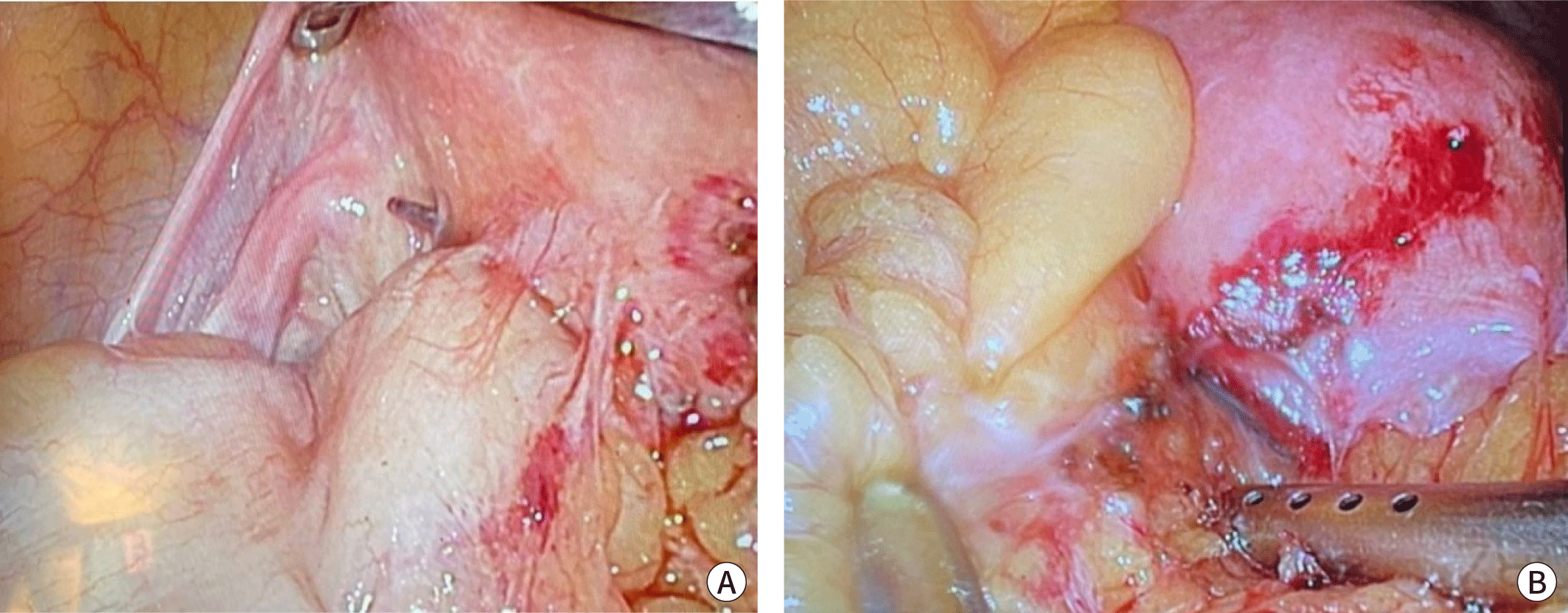
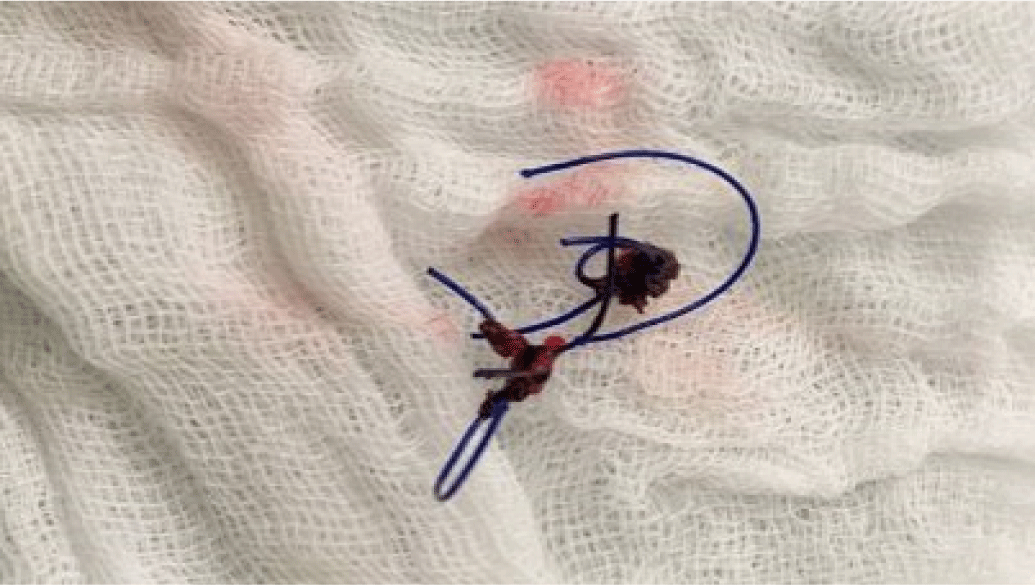
Elective laparoscopic surgery under general anesthesia was done and revealed that two non-absorbable monofilament sutures were laid on the middle and left part of the uterus, forming an adhesion between the nearby omentum and the sigmoid colon (Fig. 3A, 3B). After adhesiolysis, we recognized that one of the knots at the left uterus was penetrating the sigmoid colon. Upon removing the penetrating suture, we observed minute but definite colon wall perforation. Primary repair of the perforated colon wall was performed with continuous synthetic absorbable polyglactin sutures (Vicryl®), and the surgery was then finished. It was clearly evident that the excised suture knot was a nonabsorbable material, but the specific type of the suture material remained unknown – since we did not have access to information about the earlier surgery (Fig. 4).
The patient showed a favorable condition during the hospital course after surgery, and she was discharged on the fourth day postoperatively without any problems. After discharge, we conducted outpatient check-ups and verified that her condition continued to be stable without any gastrointestinal symptoms.
Discussion
The factors for selecting a proper suture material are the characteristics of the material, the nature of the tissue, and the surgeon’s personal preference. The main goal when choosing a suture material is for the suture to maintain the tensile strength of the wound until tissue healing provides sufficient stability. Therefore, this is an important choice for surgeons to make, and there are also fundamental recommendation for each tissue type since various tissues need different times for wound healing. In tissues such as muscles, subcutaneous tissues, and the skin, a few days are enough to heal. In contrast, fascia or tendons require weeks to months to heal; thus, several studies have indicated that absorbable sutures, which lose their tensile strength relatively slow, are superior to non-absorbable sutures. When delayed wound healing is predicted because of patient-specific factors, non–absorbable sutures are also indicated. In parenchymal organs such as the kidney or liver, a synthetic absorbable monofilament is preferable. Synthetic absorbable monofilaments can also be recommended for hollow viscous organs such as intestine or bladder, but exceptions still exist because suture selection is affected by patient characteristics, especially in patients with obesity, neoplasia, malnutrition, infection, steroid treatment, and collagen disorders.
When selecting suture materials, surgeons should keep in mind the complications that each suture could provoke. In fact, the literature contains some relevant cases of complications related to different suture types (Table 1) [4-6]. Khanal et al. [4] reported that a non-absorbable propylene suture that was used in a previous operation acted as a foreign body and led to adhesion formation [4]. The adhesion resulted in complete bowel obstruction with small bowel strangulation by constricting the band around the jejunum. The bowel strangulation was solved by removing the propylene suture and resecting the nonviable small bowel. Wang et al. [5] reported two cases of bowel obstruction and perforation caused by absorbable monofilament barbed sutures used to suture the peritoneal defect site in transabdominal preperitoneal patch surgery [5]. The obstruction was caused by a volvulus that was triggered due to an elongated tail of the barbed suture. Emergency laparoscopic exploration was performed, the embedded suture was excised and then the volvulus was solved. The second case, which involved bowel perforation, suggested that the tail of a barbed suture could penetrate the bowel wall. After the piercing barbed suture was removed, primary closure was performed at the serosal and muscular defect site. In thoracic surgery, Nakano et al. [6] reported bronchial penetration by an absorbable monofilament endoloop suture that was used for pulmonary vein ligation ; for treatment, the suture was removed [6].
| Sex | Age | Diagnosis | Operation | Outcome | Country | Reported year |
|---|---|---|---|---|---|---|
| M | 75 | Penetration of the monofilament across the wall of the bronchus | No treatment | Absorbable monofilament endoloop suture could bring out bronchial penetration. | Japan | Nakano et al., 2017 [6] |
| M | 66 | Small bowel obstruction with strangulation | Adhesiolysis and small bowel segmental resection and anastomosis | Non-absorbable propylene suture caused complete bowel obstruction | Nepal | Khanal et al., 2021 [4] |
| M | 45 | Small bowel obstruction | Removal of the embedded tail of the barbed suture from the mesentery | Bowel obstruction could be caused by an absorbable monofilament barbed suture. | Japan | Wang et al., 2021 [5] |
| M | 50 | Small bowel perforation | Removal of the tail of the barbed suture and closure of the serosal and muscular defect | Bowel obstruction could be caused by an absorbable monofilament barbed suture. | Japan | Wang et al.,2021 [5] |
In this case, we found that a non-absorbable monofilament suture caused bowel wall penetration even 15 years after the previous operation. Unlike the absorbable sutures, which are broken down by hydrolysis, non-absorbable sutures can be hidden in nearby tissue by being encapsulated or walled off by fibroblasts. Thus an adhesion could form around the nonabsorbable suture site. These adhesions may not usually lead to any symptoms, but in sporadic cases, they could induce complications such as bowel obstruction or strangulation. However if the encapsulation is not completed, the remaining suture knot could trigger another problem, such as bowel perforation, as we showed in this case report. We have summarized some remarkable cases that resulted from variable types of suture materials, and surgeons should consider a number of factors to select an optimal method for each patients. Along with personal caution, we need more education and efforts to improve awareness of the importance of deciding upon the suture material in surgery, without ignoring the complications happened that can be cause by even a tiny suture. Further research is also needed as to which suture material is better in certain circumstance and how delayed complications could be prevented after using non-absorbable suture materials.

