Introduction
With recent trends toward global aging and the increase in the sports-playing population, there has been a rise in elbow pain due to degenerative elbow diseases and sports injuries [1,2]. Minor elbow injuries can often be managed with conservative treatment, but in cases of reduced joint range due to stiffness, persistent chronic pain, neurologic deficit and instability, surgical treatment is often necessary [3]. An accurate differential diagnosis is paramount, and surgical indications need to be considered, especially for chronic elbow pain [4–6].
Lateral Epicondylitis
Lateral epicondylitis, or tennis elbow, is a common overuse injury that can significantly impact a patient's quality of life. While conservative treatment is the first line of management, some individuals may require surgical intervention when non-surgical options fail to provide relief. The extensor carpi radialis brevis (ECRB) tendon is considered to be the main anatomic structure. It commonly occurs due to repetitive wrist and forearm motions, causing microtears in the tendon, leading to pain and tenderness on the outer aspect of the elbow. While most cases of lateral epicondylitis can be successfully managed with conservative treatments, such as rest, physical therapy, and anti-inflammatory medications, some patients may not respond adequately to non-surgical approaches.
Surgical intervention is typically considered when conservative treatment has failed to provide relief, and patients continue to experience debilitating symptoms that significantly impact their daily activities after appropriate non-surgical management for 3 months.
Surgical options include arthroscopic ECRB release (Fig. 1), open release with or without ECRB repair and percutaneous tenotomy [7]. Both arthroscopic and open surgical procedures for lateral epicondylitis have shown satisfactory outcomes in relieving pain and restoring function. In the recent literature, the arthroscopic treatment of lateral epicondylitis has shown favorable results, with reduced postoperative pain and faster recovery compared to open procedures. Most patients experience significant improvement within several weeks after surgery, with full recovery taking several months. Rehabilitation, including physical therapy, stretching, and strengthening exercises, is essential for restoring elbow strength and range of motion (ROM).
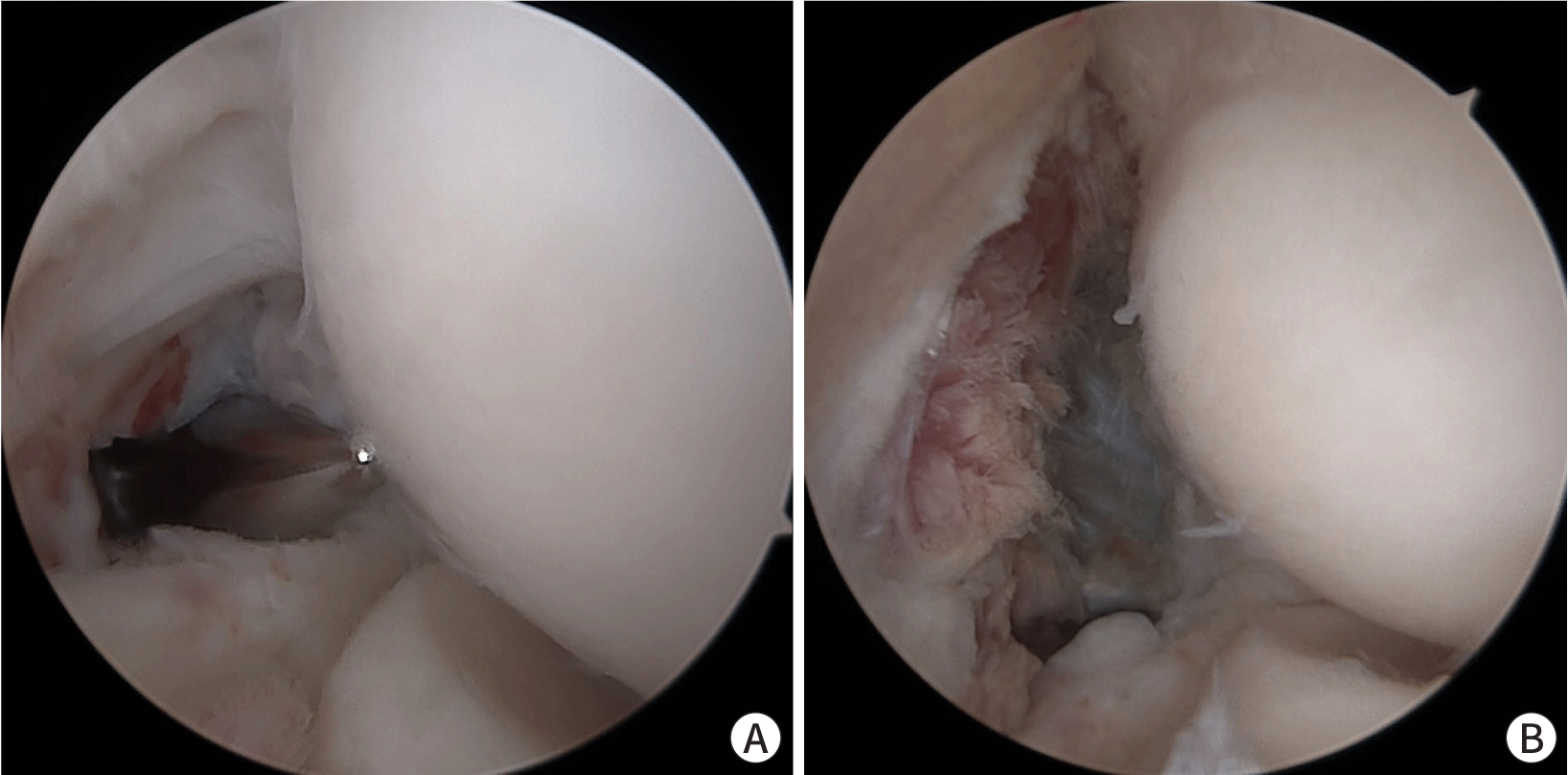
The surgical approach should be chosen based on the severity of the condition, patient-specific factors, and the surgeon's expertise. A prompt diagnosis, appropriate surgical planning, and thorough rehabilitation are essential for achieving successful outcomes. Further research and long-term follow-up studies are necessary to optimize surgical techniques and improve patient satisfaction in the management of lateral epicondylitis.
Due to the anatomical proximity of the ECRB tendon and the lateral collateral ligament (LCL) complex, care must be taken during surgery to avoid unnecessary damage to the LCL complex [8,9]. In cases of LCL complex insufficiency, which is often found as a concomitant lesion in patients with chronic recalcitrant tennis elbow, if instability is observed before surgery, it may be possible to perform LCL complex repair or reconstruction during surgery [10,11].
Medial Epicondylitis
Medial epicondylitis, or golfer's elbow, is an inflammatory condition that affects the tendons of the forearm muscles, which are the wrist flexor and pronator, attached to the medial epicondyle of the elbow. The repetitive use of these muscles can lead to microtears and degeneration of the tendon, causing pain and tenderness on the inner aspect of the elbow. While most cases of medial epicondylitis respond well to conservative treatments, such as rest, physical therapy, and anti-inflammatory medications, surgical intervention may be necessary for patients who do not achieve satisfactory relief.
Surgical treatment is typically considered when relief is not achieved after more than 3 months of conservative treatment, and patients continue to experience significant pain and functional limitations. In rare cases, ulnar nerve symptoms may also be present, for which surgical management should be considered.
As with lateral epicondylitis, both open and arthroscopic procedures for medial epicondylitis have shown favorable outcomes in relieving pain and restoring function. Arthroscopic procedures can have technical dependency due to limited visualization from the lateral viewing portal [12]. The main aim is to release the flexor tendon with the pronator group of the elbow. The surgical technique includes cortical bone resection and lengthening using pie crusting technique after release of the flexor tendon group (Fig. 2). Most patients experience significant improvement within several weeks after surgery, with full recovery taking several months.
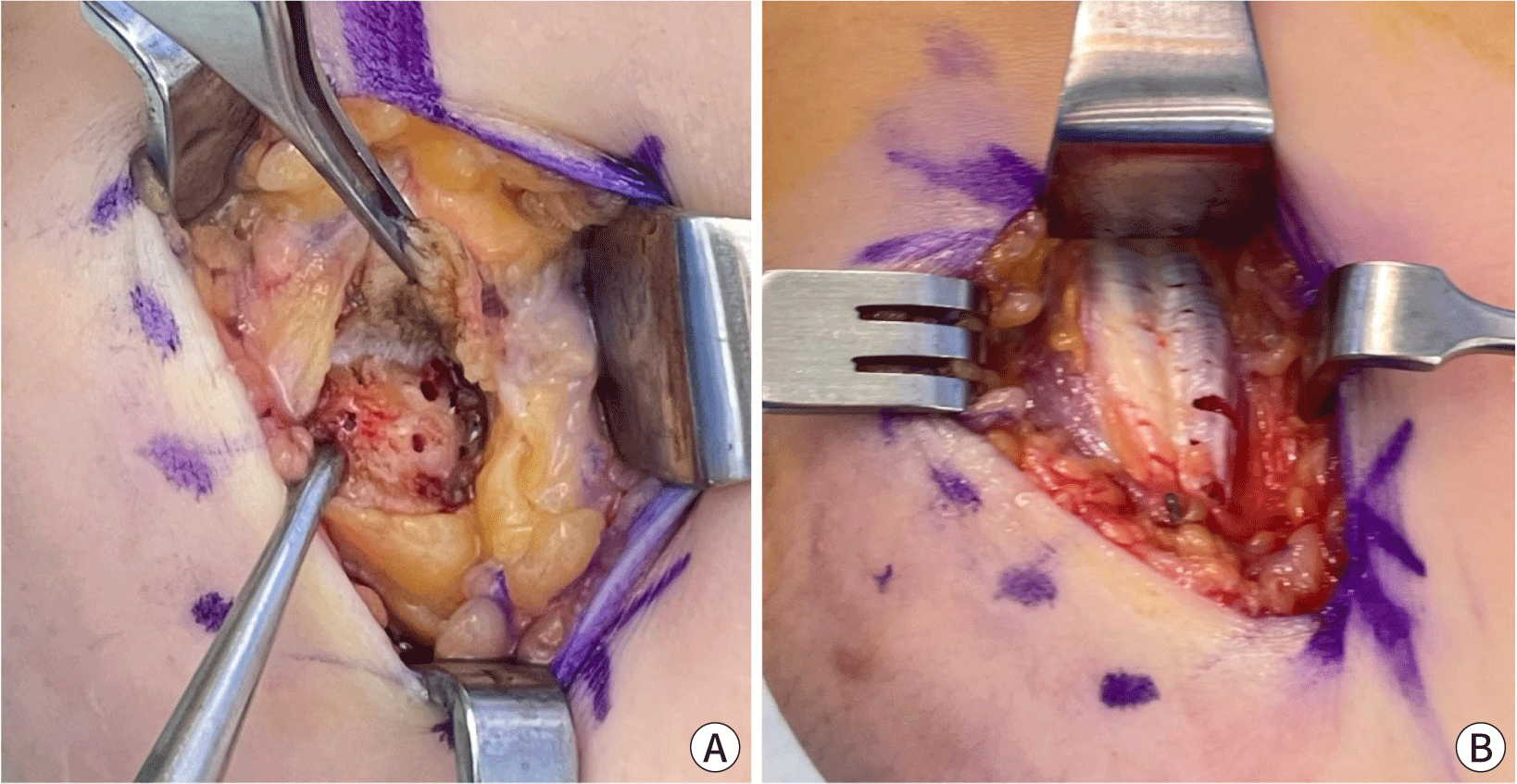
Due to the close anatomical proximity to the ulnar nerve, there is always the possibility of nerve damage; therefore, it is essential to routinely check the course of the nerve during surgery. During incision surgery, the course is verified, and decompression is performed as needed if symptoms of pressure on the spinal nerve are suspected. During the release, care should also be taken to avoid damaging the ulnar collateral ligament [13].
Pathologic Plica Syndrome
Elbow plica syndrome is a condition in which the synovial folds within the elbow joint become inflamed and hypertrophic, leading to painful symptoms and functional impairment [14]. When conservative treatment fails to provide relief, surgical intervention is often necessary [15]. Two common surgical approaches for elbow plica excision are open surgery and arthroscopic plica excision. This section compares these two techniques to help orthopedic surgeons make informed decisions regarding the optimal surgical approach for patients with elbow plica syndrome [16].
Surgical excision of pathologic plica is typically considered when the elbow plica is large and fibrotic, which could cause plica snapping or be associated with other intra-articular pathologies. This allows a more extensive view of the joint and facilitates concurrent management of any coexisting conditions [16].
Both open surgery and arthroscopic plica excision are effective treatment options for elbow plica syndrome, each with its advantages and disadvantages [17]. Open surgery allows more direct visualization of the antero-lateral plica and any additional abnormalities, potentially enabling improved resolution of symptoms. Patients typically experience immediate relief from preoperative symptoms, with progressive improvement over several weeks. Arthroscopic plica excision is preferred for both anterolateral and posterolateral plica with significant intra-articular pathologies. This is a minimally invasive procedure that enables better preservation of the surrounding tissues (Fig. 3). Arthroscopic plica excision reduces surgical trauma, leading to a quicker recovery and less postoperative pain.
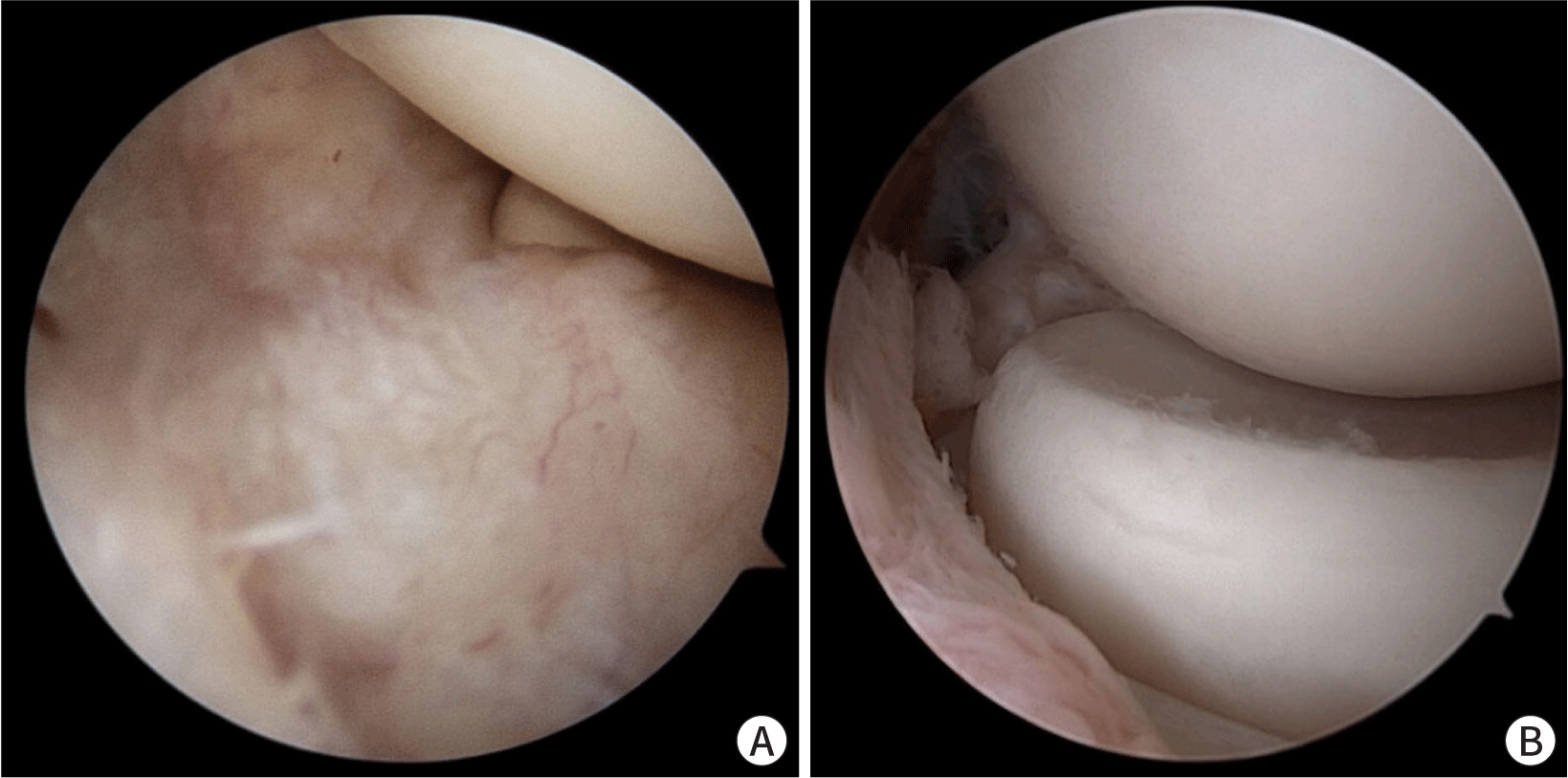
The choice of surgical approach should be based on the size and extent of the plica, the presence of concomitant intra-articular pathologies, surgeon expertise, and patient-specific factors. A thorough evaluation and informed decision-making process will lead to successful outcomes and improved patient satisfaction. Further research and comparative studies are warranted to refine surgical techniques and improve patient outcomes in the surgical treatment of elbow plica syndrome.
The pathologic plica is primarily located around the radial head, extending from the front to the back. In particular, when excising the front plica, one must be fully aware of the course of the radial nerve to prevent injury to the radial nerve during surgery [18].
Elbow Osteoarthritis
Elbow arthritis is a progressive degenerative condition that affects the articular surfaces of the elbow joint, leading to pain, swelling, and limited joint mobility. It can result from various causes, including age-related wear and tear, post-traumatic injuries, or inflammatory conditions such as rheumatoid arthritis. While conservative treatments, such as pain management, physical therapy, and activity modification are commonly employed in early-stage arthritis, surgical intervention becomes necessary when non-surgical measures fail to provide adequate relief.
Patients with osteoarthritis often experience their first symptoms around the age of 50, and this illness disproportionately affects men, with a male-to-female ratio of 4:1. Osteoarthritis is more typically found in the dominant extremity. Patients with elbow arthritis commonly complain of pain, weakness, and loss of motion.
-
- Loss of motion: The functional ROM required for daily living activities is 100° (30° of extension to 130° of flexion) and a 100° arc of forearm rotation (50° of pronation to 50° of supination). The main pathologic mechanisms causing motion loss include capsular contracture and osteophytes in the fossa, as well as processes of the olecranon and coronoid.
-
- Impingement discomfort (endpoint pain): Patients frequently experience pain at the end of motion in flexion and extension. Radiologic findings show that the three-dimensional matching of shape in the olecranon and coronoid fossa and process has been destroyed, with point contact leading to osteophyte growth. The concentration of contact force at the place of contact could be an explanation, although the cause of impinging discomfort remains unknown.
-
- Discomfort at rest or in the mid-arc: Some patients report discomfort in the mid-arc of motion or even at rest. This sort of discomfort is caused by cartilage erosion or destruction, which is common in severe elbow arthritis. If the discomfort is modest or inconsistent, using elbow mobility with axial loading as a provocative test may be beneficial.
Because the most common symptoms of elbow osteoarthritis include resting discomfort, mid-arc pain from joint cartilage breakdown, endpoint pain, and reduced ROM from spurs and loose bodies, a staging system or classification for elbow arthritis should incorporate symptom-related variables to guide treatment. The Broberg and Morrey classification and the Hastings and Rettig classification have been used for qualitative staging to identify illness severity. [19] The Broberg and Morrey classification is based on osteophyte formation and narrowing of the joint space. The Hastings and Rettig system is based on the presence of subluxation and radiocapitellar joint involvement.
A CT-based staging technique, or Kwak’s classification, quantifies spurs in the fossa by assessing the involved depth on sagittal CT slices [20]. An "involved fossa" is defined as more than 50% involvement of the fossa. “Joint space narrowing” is defined as the presence of a gap of more than 1 mm in the ulnohumeral joint in more than 50% of the joint space in the reference section. A lack of involved fossa with intact joint space is defined as grade 0, a uni-compartmentally involved fossa with an intact ulnohumeral joint space is defined as grade 2, and joint space narrowing regardless of the state of the fossa is defined as grade 3 (Fig. 4). CT-based staging is more therapeutically practical and reproducible than prior plain radiograph-based staging techniques.
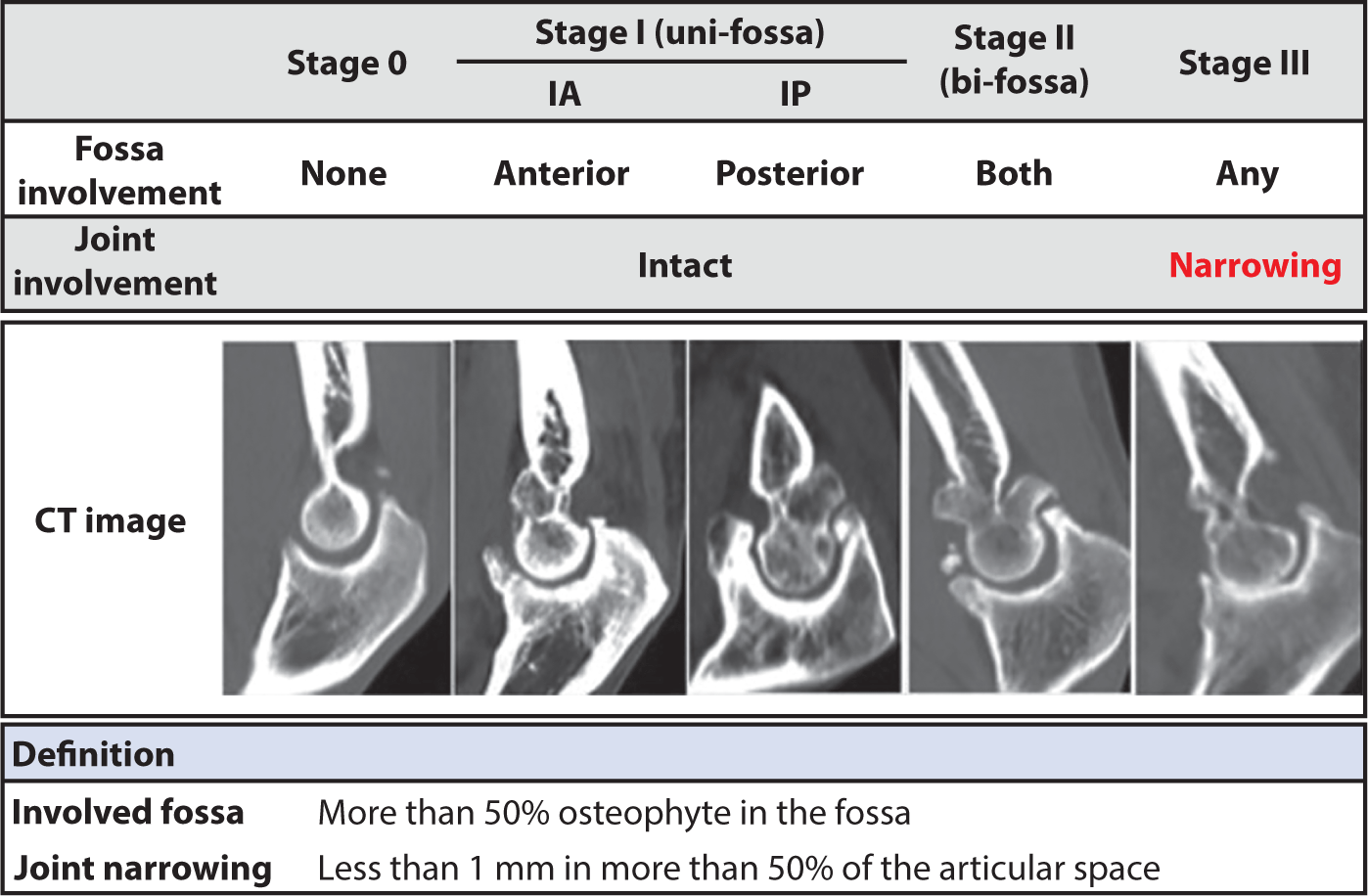
The most common reason for arthroscopic osteocapsular arthroplasty (OCA) is functional loss of elbow motion and impingement pain caused by osteophytes and capsular tightness [21]. The rationale for surgery is uncomfortable impingement or functional impairment due to the necessity for terminal elbow extension in patients with a functional arc of motion, which is defined as flexion from 30° to 130° preoperatively. This indication does not apply to every patient. Although most people may go about their daily lives with a functional arc of motion in their elbow, young and high-demand patients (often athletes) cannot tolerate smaller degrees of contraction. Low radiologic grades with apparent symptoms (e.g., impingement discomfort and mechanical symptoms of loose bodies) can also be evaluated. Arthroscopy can be used to treat less severe contractures in these patients.
End-stage elbow osteoarthritis can be considered a relative contraindication because it is associated with poor clinical and radiologic outcomes. However, even for advanced elbow osteoarthritis, elbow debridement or OCA is still an option as a palliative treatment for patients who refuse total elbow arthroplasty (TEA) or are not good candidates for TEA due to infection. Significant anatomic deformity is a contraindication. Depending on the surgeon's experience, prior submuscular transposition of the ulnar nerve may be a selective contraindication. Contraindications do not include ulnar nerve dislocation or prior subcutaneous transposition, unsuccessful prior contracture release, or significant scarring from skin grafts or flaps.
Open elbow debridement, a procedure that involves removing the diseased or damaged tissue and smoothing out the remaining joint surfaces by eliminating osteophytes, the adhesive capsule, and loose bodies, has been a traditional approach to treating elbow osteoarthritis. It is generally recommended for severe osteoarthritis that needs severe adhesiolysis, and the elbow requires ulnar nerve management.
The arthroscopic approach has emerged as an appealing alternative for addressing both mechanical impingements caused by osteophytes and soft tissue contracture as less invasive surgical techniques have advanced (Fig. 5). The advantages of arthroscopic OCA include little surgical damage, which encourages faster rehabilitation and minimizes the likelihood of capsular contractures by lowering the morbidity associated with a long incision and joint exposure.
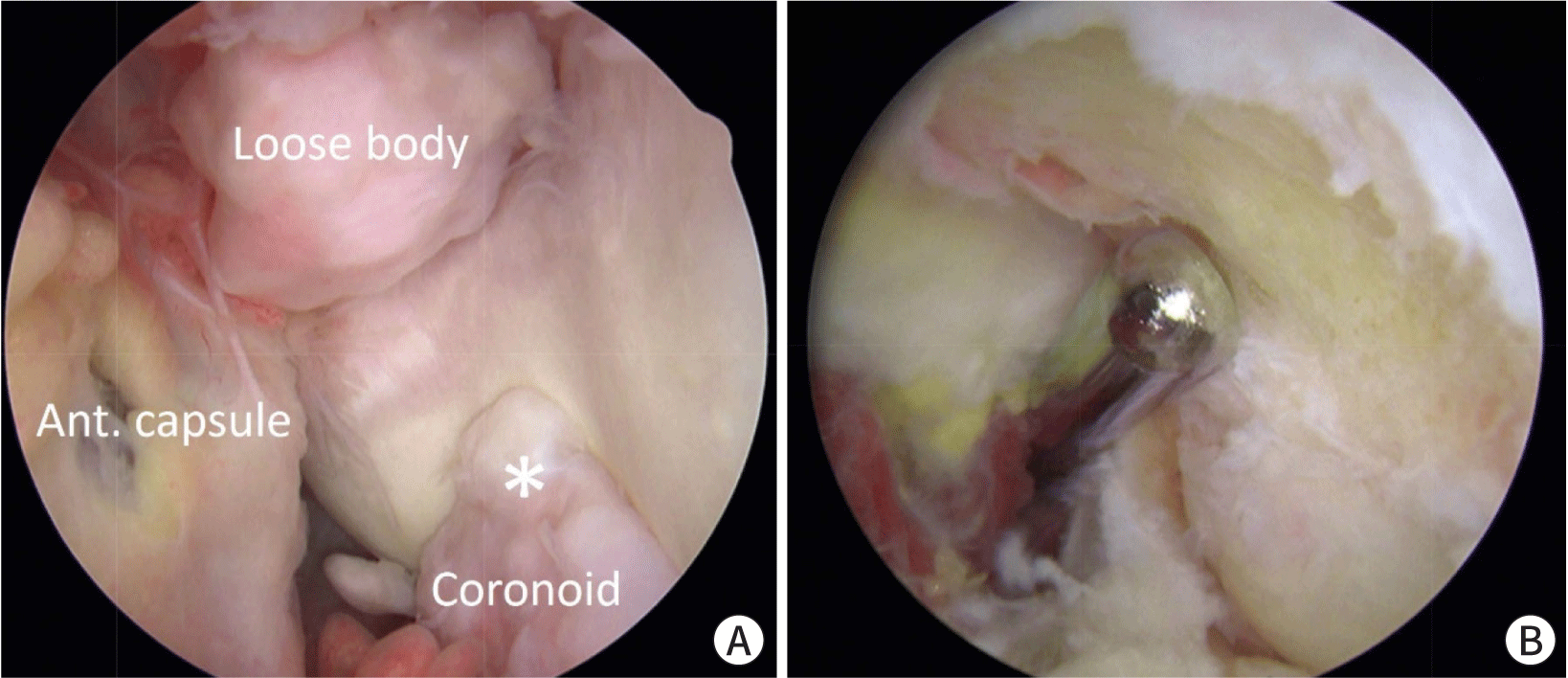
Both arthroscopic and open surgical techniques have shown positive outcomes in treating elbow arthritis [21–23]. With positive clinical outcomes for pain alleviation and ROM recovery, open debridement has been extensively performed and recommended by many qualified surgeons. It has been proposed that whatever functional restoration or symptom reduction that can be obtained through open surgery can be fully attained through arthroscopy. A recent study also found that arthroscopic OCA had comparable clinical outcomes, reaching the significant conclusion that neither technique can ensure excellent outcomes in patients with advanced osteoarthritis. Kim et al. found in a comprehensive analysis that both open and arthroscopic OCA enhanced ROM and clinical ratings, but that open debridement had higher complication and reoperation rates than arthroscopic OCA. However, arthroscopic OCA is more technically difficult than open surgery, and training and knowledge of the procedure are required to avoid neurovascular damage.
After restoring elbow motion, delayed-onset ulnar neuritis (DOUN) may arise. DOUN has been observed to occur in 11% of cases following elbow arthroscopic contracture release [24]. The three clinical presenting patterns are rapidly progressive, non-progressive, and slowly progressive [25]. The most prevalent pattern that necessitates an urgent reoperation for nerve management is the rapidly progressing pattern, which is characterized by increased discomfort in the cubital tunnel, progressive loss of elbow motion, and neuropathy. If ulnar nerve transposition is delayed for more than 2 weeks following surgery, there is no complete return of neurological function. Preoperative hypertrophic ossification, preoperative neurological complaints, and the preoperative arc of motion are all connected with an elevated risk of DOUN. Before treatment, we advocate for restricted open ulnar nerve decompression while maintaining a high index of suspicion and avoiding end-range stretching if it generates symptoms such as ulnar neuritis or discomfort around the cubital tunnel.
TEA was initially created to treat advanced rheumatoid arthritis, but its indications have since been expanded to include unfixable comminuted fractures, post-traumatic arthritis, and primary osteoarthritis [26,27]. Because TEA is seldom performed, most surgeons have less experience with it than with hip and knee arthroplasty, and limited long-term outcome data are available. To avoid making unnecessary errors, surgeons must learn about this surgery by carefully examining previous literature [28–30].
Osteochondritis Dissecans
Osteochondritis dissecans (OCD) of the capitellum is an articular cartilage and subchondral bone disorder that primarily affects juvenile gymnasts and overhead athletes such as baseball and tennis players [31]. This disease is thought to be caused by recurrent loading at the comparatively weakly vascularized capitellum. Stable lesions may produce pain during and after physical exercise in the early stages. Advanced (unstable) lesions, in which the cartilage has separated, and loose bodies have formed, can cause considerable pain, loss of motion, and locking of the elbow joint, eventually leading to the termination of athletic activity. Rest, analgesics, and physical therapy are advised for early-stage lesions in skeletally immature patients, whereas surgical treatment is recommended for advanced symptomatic lesions.
Arthroscopic treatment is generally recommended for stable OCD lesions that have not progressed to severe cartilage damage or loose body formation. This technique is less invasive and allows better visualization and treatment of early-stage lesions. Open surgery is considered for more advanced OCD lesions, particularly those with loose bodies or extensive cartilage damage that may not be amenable to arthroscopic treatment.
Surgical intervention plays a vital role in managing elbow OCD when conservative treatments are insufficient. Both arthroscopic and open surgical techniques have shown positive outcomes in treating this condition, with each approach having its specific indications and advantages.
Arthroscopic debridement and microfracture for advanced capitellar OCD have favorable clinical outcomes in terms of pain, function, ROM, and comorbidities, particularly in patients with an open growth plate, loose body removal, and shorter duration of symptoms. However, given that only 62% of our patients returned to their major sport, a more active strategy may be required for high-level athletes who want to return to their pre-injury level [32]. Open surgical procedures for elbow OCD can also be effective in cases with more significant cartilage damage and loose bodies. Patients may experience a more prolonged recovery compared to arthroscopic surgery, and rehabilitation is crucial for regaining elbow function. Long-term outcome studies are needed to show whether the improved clinical outcomes of arthroscopic debridement and microfracture are sustained.
The choice of surgical technique should be based on lesion stability, cartilage damage extent, patient age, activity level, and surgeon experience. Early diagnosis and appropriate surgical management can lead to successful outcomes and the preservation of elbow function for patients with OCD. Further research and long-term follow-up studies are necessary to optimize treatment strategies and enhance patient satisfaction in the surgical treatment of elbow OCD.
Nerve Entrapment Syndrome
Elbow radial tunnel syndrome is a nerve entrapment disorder that involves the compression or irritation of the radial nerve within the radial tunnel, situated beneath the supinator muscle [33]. The condition of irritation or compression of posterior interosseous nerve can lead to persistent forearm pain and sensory disturbances along the dorsal aspect of the hand [34,35]. When conservative treatments, such as rest, physical therapy, and anti-inflammatory medications, fail to alleviate symptoms, surgical intervention may be necessary. Surgical decompression is considered when conservative measures have been ineffective, and the patient experiences persistent pain, functional limitations, or progressive neurological deficits [36]. The procedure aims to relieve the pressure on the compressed radial nerve within the radial tunnel. Surgical decompression of the radial nerve in the radial tunnel has shown promising results, with most patients experiencing a reduction in pain and improved function. Sensory disturbances and weakness tend to improve gradually after surgery [37].
Elbow cubital tunnel syndrome is a neurological condition characterized by the compression of the ulnar nerve as it travels through the cubital tunnel, which is located on the medial aspect of the elbow [38]. Entrapment can lead to various symptoms, including pain, tingling (paresthesia), weakness, and numbness in the hand and forearm (Fig. 6). When conservative treatments, such as activity modification, splinting, and anti-inflammatory medications, fail to alleviate symptoms, surgical intervention may be necessary. This section explores the various surgical options for elbow cubital tunnel syndrome, assisting orthopedic surgeons in making informed decisions regarding the management of this condition.
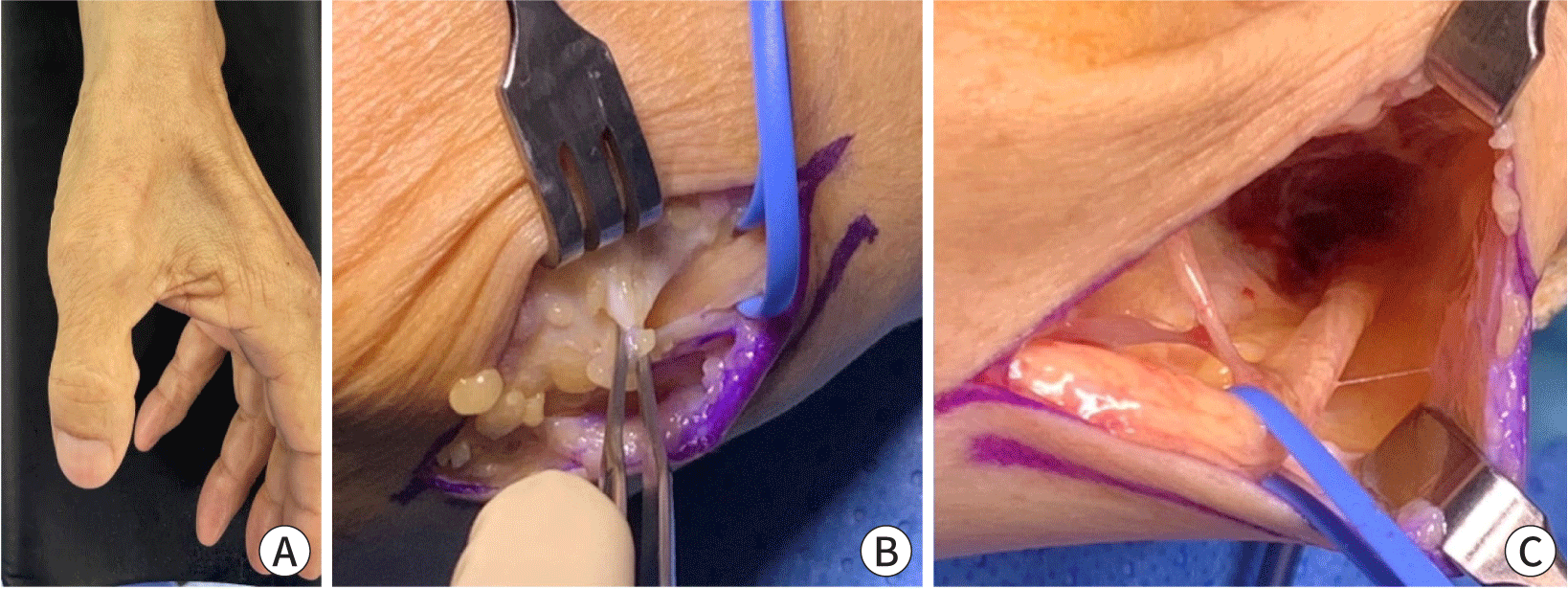
Surgical options include ulnar nerve transposition, medial spondylectomy, or simple decompression. The chosen method depends on the severity, anatomical considerations, and the surgeon's preference and experience. Postoperative care, involving physical therapy and close monitoring, is essential to ensure nerve recovery and functional restoration. A comprehensive review of both surgical techniques and postoperative care strategies reveals a generally favorable prognosis with a low complication rate. Tingling, weakness, and numbness tend to improve gradually after surgery depending on disease severity and disease period [39]. Successful surgical outcomes rely on a prompt diagnosis, accurate localization of the entrapment site, and meticulous surgical technique. Careful patient selection and thorough preoperative evaluation are essential to achieve favorable results and minimize potential complications.

