Introduction
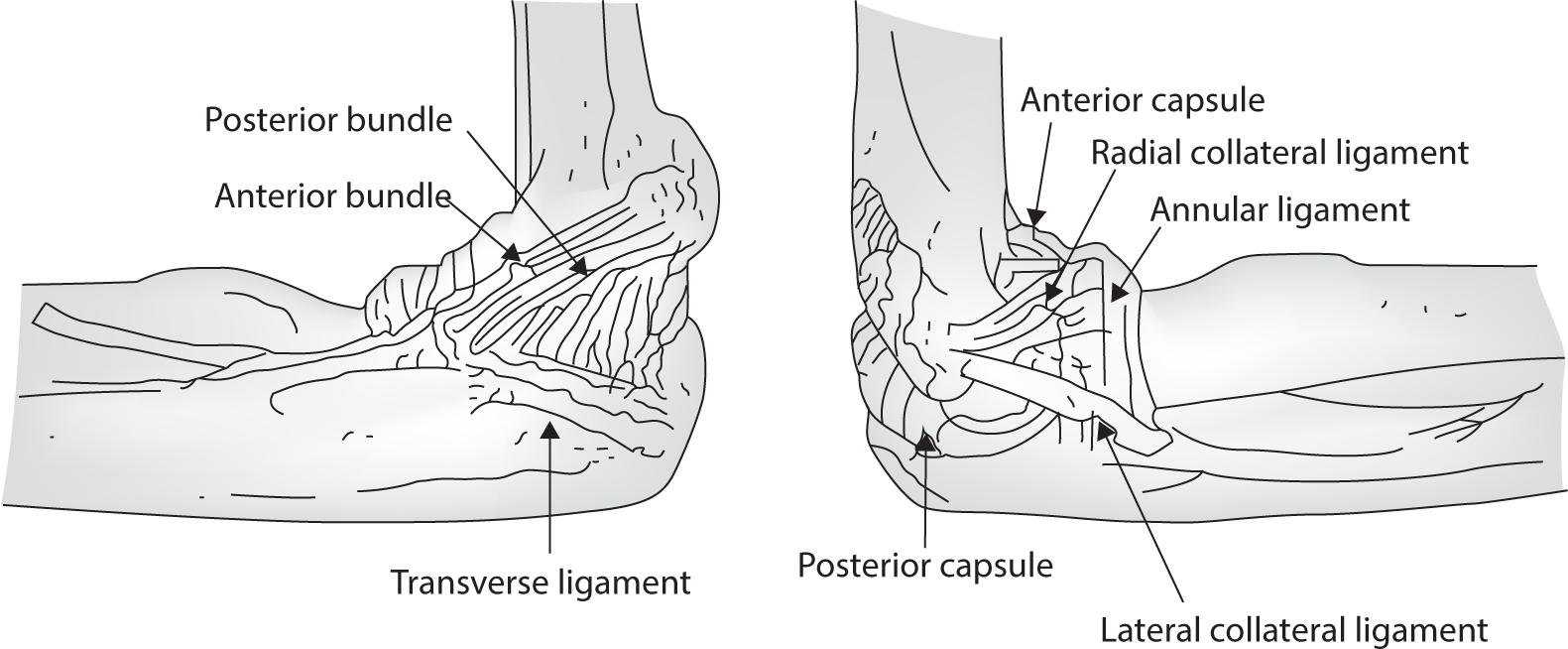
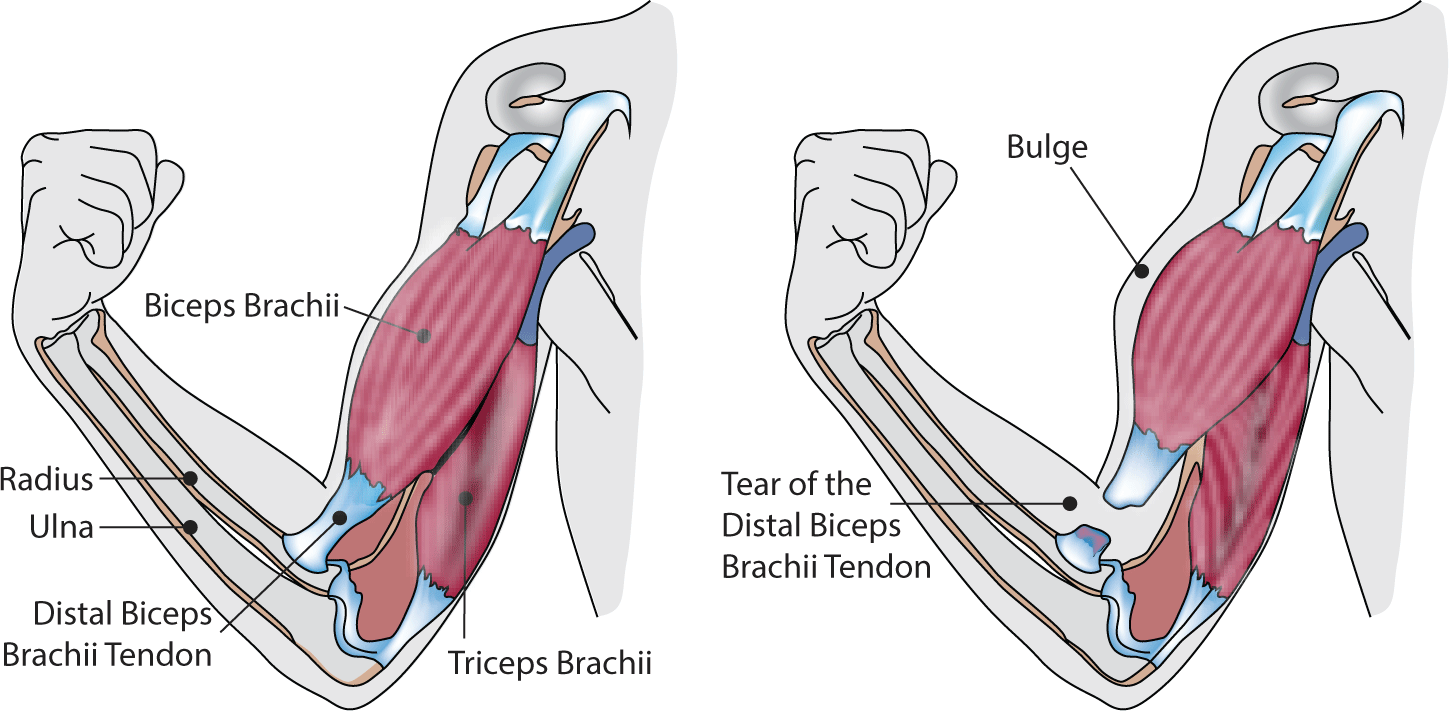
The elbow joint is a complex structure, comprised of two distinct joints: the ulno-trochlear joint and the radio-capitellar joint. The ulno-trochlear joint functions as a hinge, while the radio-capitellar joint operates as a limited ball-and-socket joint. As a result, the elbow joint is capable of two types of motion: flexion/extension and supination/pronation. Furthermore, the elbow joint is encased by a joint capsule and ligaments, which include the lateral ulnar collateral ligament and radial collateral ligament in the lateral compartment, and the medial collateral ligament in the medial compartment. The joint is also surrounded by muscles, such as the extensor/flexor, biceps tendon, and triceps, as well as joint fluid. Pathologies of these complex anatomical structures can potentially induce elbow joint pain (Fig. 1) [1–3].
While most elbow pathologies can be effectively addressed with various conservative treatments, patients experiencing persistent pain or compromised function may require surgical intervention. Common causes of elbow joint pain that necessitate surgery include epicondylitis (medial and lateral), osteoarthritis (degenerative/post-traumatic), biceps/triceps tears, and neuropathy (ulnar/radial) [4–9]. Additionally, it is challenging for surgeons to achieve satisfactory clinical outcomes for fractures near the elbow joint. Although most patients who undergo surgery for the aforementioned causes have acceptable results, there are potential complications, such as stiffness, residual pain, decreased function, and exacerbated neuropathy [10–13]. These complications can be minimized—and the need for additional surgery could potentially be eliminated—if patients receive appropriate postoperative rehabilitation based on correct principles.
Therefore, we reviewed previous studies on postoperative rehabilitation for various pathologies or surgical procedures of the elbow joint. We discuss the principles of postoperative rehabilitation for the elbow joint, drawing from recently published articles. We hope to provide suggestions that will be accessible and useful to clinicians, even those with limited experience in orthopaedic surgery.
General Principles
The objective of elbow rehabilitation is to restore optimal function without pain, while taking into account the patient's anatomical and physiological limitations. To achieve successful rehabilitation, practitioners should adhere to the following guiding principles: 1) make a comprehensive and accurate diagnosis, 2) manage and alleviate pain and swelling, 3) start gentle motion exercises early on, 4) reestablish neuromuscular stability around the elbow, 5) consider the entire kinetic sequence when approaching elbow rehabilitation, and 6) assist the patient in returning to their preoperative level, whether that involves sports or simply everyday tasks [14].
The general principles of elbow fracture management are as follows [15,16]:
-
- Week 1−2: Protect and stabilize the wound by decreasing swelling. A gentle passive range of motion can be allowed under a clinician’s guidance. During this period, hand and shoulder motion is recommended.
-
- After 2 weeks: If the wound is stable, the stitches can be removed. If not, stitch removal can be delayed until 3 weeks.
-
- Weeks 2−6: Conduct physical therapy to improve the range of motion with assisted active and passive motion exercises.
-
- Week 6: Increase the intensity of range of motion exercises, using active motion exercises.
Rehabilitation after Common Elbow Surgery Procedures
Lateral epicondylitis, also known as “tennis elbow,” is an overuse injury that affects the wrist extensor muscles. These muscles include the extensor carpi radialis brevis, extensor digitorum communis, and extensor carpi radialis longus, and the injury occurs at their insertion on the lateral epicondyle. Medial epicondylitis, also referred to as “golf elbow,” is characterized by chronic tendinosis of the flexor-pronator musculature at its insertion on the medial epicondyle of the humerus, resulting from overuse or repetitive stress. Surgical treatment is considered after other conservative treatments have been tried. These treatments include medication with NSAIDs, physical therapies, strengthening exercises for the extensor/flexor muscles with counterforce braces, injection therapy (which may include steroids, autologous blood, polydeoxyribonucleotide, or platelet-rich plasma), and extracorporeal shockwave therapy [17–23]. Open, percutaneous, or arthroscopic approaches to tendinopathy, involving release and debridement, have shown excellent outcomes in resolving chronic, recalcitrant elbow pain and functional disability [17,24]. However, returning to work and restoring the normal range of motion in the elbow joint, as well as grip strength, can only be achieved following essential postoperative rehabilitation. This rehabilitation should involve active physical therapy, including eccentric strengthening exercises.
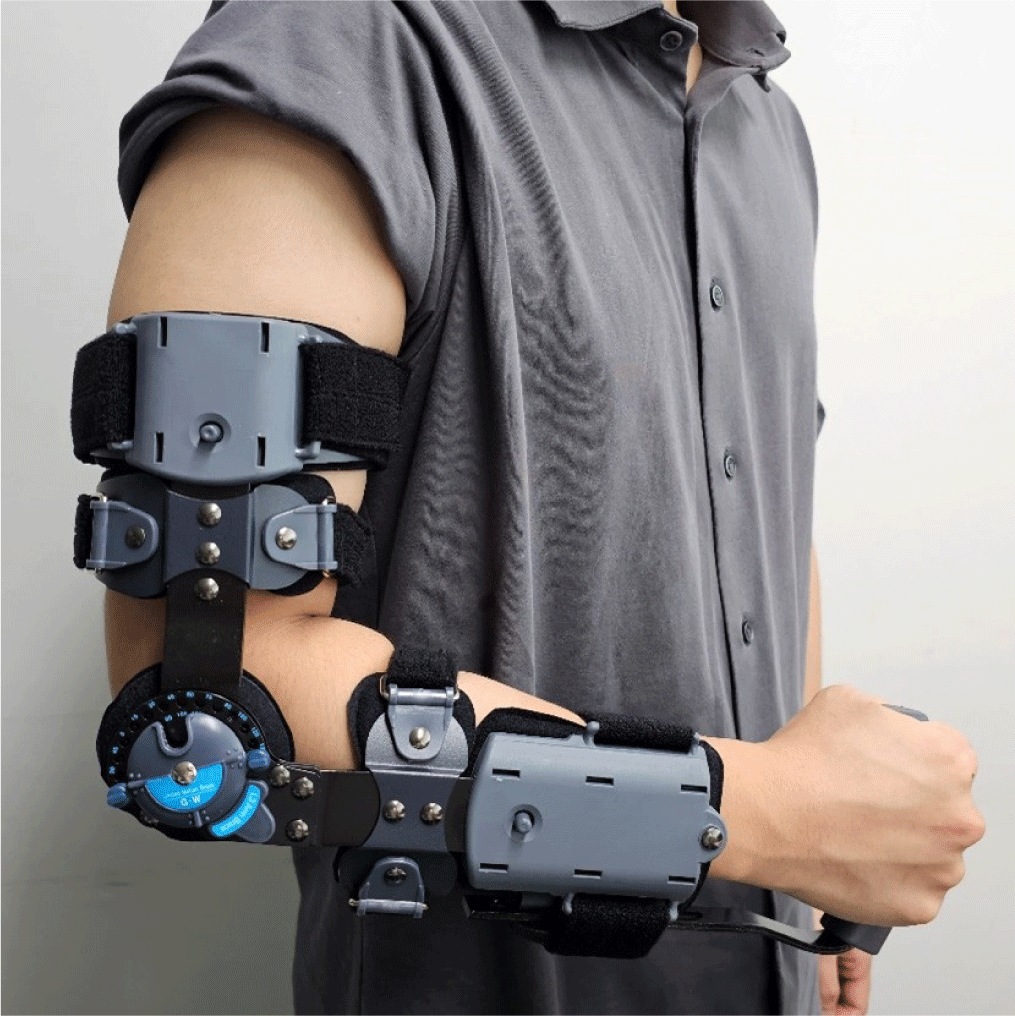
The general principles for postoperative rehabilitation in lateral and medial epicondylitis are identical. These often involve periods of protection, active physical therapies, and strategies to restore the full range of motion and strength in the elbow. Rehabilitation following a ligament repair typically necessitates a longer protection period, often requiring the use of a removable static splint for up to 2 weeks (Fig. 2). For managing postoperative swelling and pain, icing, elevation, and compression can be utilized. NSAIDs or other prescribed pain medications may also be recommended. After 2 weeks, controlled mobilization and isometric strengthening exercises are progressively introduced. Clinicians should encourage patients to mobilize the affected elbow side, which includes flexion and extension in the forearm's neutral position. Depending on the surgeon's guidelines, gentle passive and active assisted range of motion exercises can commence. Gradual progression of these exercises helps restore flexibility and prevent joint stiffness. Additionally, isometric exercises, where the muscle contracts without moving the joint, can begin. These are followed by isotonic exercises, which involve joint movement. At this point, patients can start light daily activities, ensuring no pain is elicited. Six weeks post-surgery, functional exercises and eccentric strengthening exercises, where the muscle lengthens under tension (like slowly releasing a weight), can be particularly effective for tendinopathies and can be initiated. Physiotherapy is prescribed if any residual stiffness in the elbow is noticed. Depending on the patient's goals, specific exercises mimicking daily or sporting activities can be started. Physical therapists may also use ultrasound, electrical stimulation, or laser therapy to promote healing and reduce pain. Full recovery to sports or work is typically expected between three to six months [24,25].
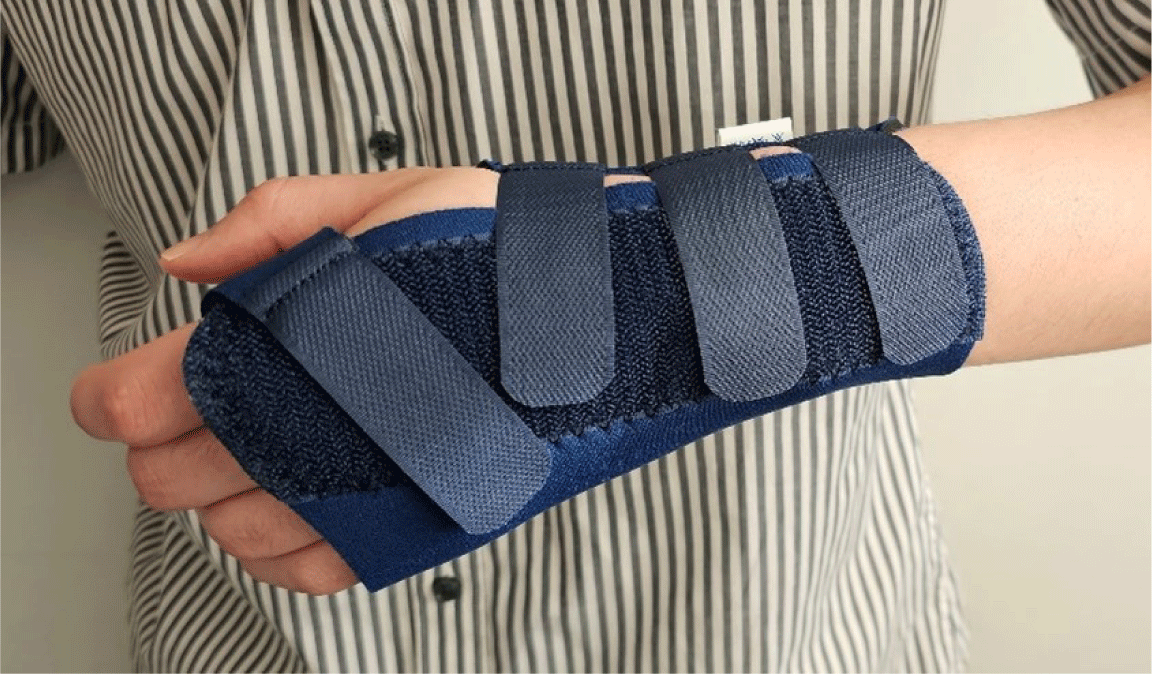
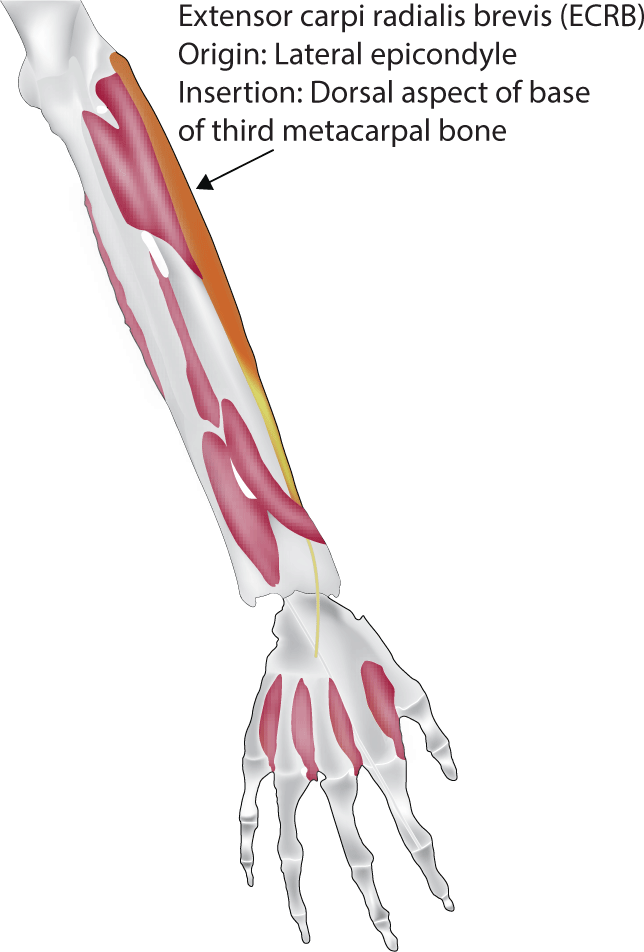
During the recovery process, a counterforce brace treatment just distal to the elbow and a cockup wrist splint can be recommended to reduce the load at the operative site (Fig. 3). The wrist splint is required to protect the extensor carpi radialis brevis, which inserts at the base of the third metacarpal bone (Fig. 4). Rehabilitation following debridement usually involves a shorter protection period, with an earlier introduction of mobilization exercises to prevent stiffness and adhesions. Recovery from open surgery often requires longer immobilization to ensure wound healing and to minimize stress on the repaired or treated structures (Fig. 5). Physical therapy, initially focusing on gentle range of motion exercises, is crucial. For arthroscopic surgery, which involves smaller incisions and minimal soft tissue disruption, faster rehabilitation is often permitted. Patients may initiate range of motion exercises sooner, and strengthening exercises may be introduced earlier than after open surgery.
Since the elbow joint is not weight-bearing, osteoarthritis is not as common as in other joints. However, the elbow bears the load created by gravity and muscle contracture in dynamic swing movements [26]. For this reason, degenerative arthritis frequently develops in individuals who engage in heavy manual labor, rely on crutches, or are overhead-throwing athletes [27]. Recently, surgical procedures such as open or arthroscopic osteo-capsular arthroplasty have been commonly performed to alleviate primary symptoms associated with osteoarthritis. These symptoms include pain at the terminal range of motion, mechanical symptoms (such as impingement, locking, and crepitus), and stiffness [28]. The procedures involve steps such as capsular release, synovectomy, and the removal of osteophytes and loose bodies, all aimed at reducing pain and increasing range of motion [29].
The clinical outcomes after surgical treatment for osteoarthritis are largely influenced by postoperative management. One of the primary objectives of these treatments is to regain the range of motion, ideally achieving a functional range of motion of 30°−130° in extension-flexion and 50° in pronation-supination. Initially, a soft compressive dressing is applied after the surgical procedures. This dressing is replaced with a simpler one on the first postoperative day, and patients are taught to perform active assisted range of motion exercises with help from the contralateral hand (Fig. 6). Upon discharge, patients are encouraged to move their elbows within a comfortable range and are instructed to continue practicing range of motion exercises at home for a period of 3 months. Nighttime splinting is recommended during the first 3−4 weeks post-surgery. The home rehabilitation regimen involves completing full extension and flexion exercises ten times consecutively, with a 10-second pause between each repetition, six times daily [29,30]. Telehealth and YouTube have proven to be valuable educational resources for rehabilitation, with patients often expressing satisfaction with their usefulness. Telehealth, in particular, offers a platform for real-time interaction between patients and healthcare professionals, facilitating guided exercise demonstrations, immediate feedback, and personalized adjustments to rehabilitation plans. Conversely, YouTube provides a wealth of video tutorials and demonstrations related to rehabilitation exercises. These videos typically include step-by-step instructions, common pitfalls to avoid, and variations to accommodate different levels of mobility and strength. Given their detailed guidance and accessibility, both telehealth and YouTube are highly recommended as effective tools to support and enhance the home rehabilitation process [31,32].

In cases where traditional treatments or other joint-preserving procedures fail to yield positive results, and individuals continue to suffer from symptoms such as pain during specific ranges of motion, discomfort during flexion and extension, and persistent pain even at rest or during the night, total elbow arthroplasty (TEA) may be considered. However, before deciding on this surgical intervention, it is crucial for individuals to understand and consent to the activity limitations that come with a TEA. Following the procedure, standard postoperative care for TEA is implemented. The operated arm is typically immobilized using a splint for a few days to a week, depending on the condition of the extensor mechanism and the surrounding tissues. When the arm is not in the splint, periodic active or passive elbow movements are encouraged. By the end of six weeks, the use of the removable splint is typically discontinued. After surgery, patients are generally advised to avoid repetitively lifting anything over 1 kg and to limit lifting anything over 5 kg to rare occasions [33–35].
Cubital tunnel syndrome is the second most common type of peripheral neuropathy in the upper extremity [36]. Chronic ulnar nerve neuropathy may lead to a loss of sensation, muscle weakness or atrophy, and joint contractures. While non-surgical management may be indicated for mild cases of cubital tunnel syndrome, surgical intervention is typically pursued for more advanced cases. Numerous types of procedures are available, including in situ decompression and or ulnar nerve anterior transposition, which can be submuscular, intramuscular, or subcutaneous.
Postoperative care and rehabilitation can vary based on the surgical method used. For in situ decompression, a bandage is used for protection for at least 2 days. The patient is permitted to move their elbow immediately. For patients who undergo ulnar nerve anterior transposition, additional protection may be necessary. This often involves the use of a removable splint at night for the first 2 weeks. The initial phase, which lasts 7−10 days, requires patients to refrain from elbow range of motion activities, particularly full extension. During this time, a posterior splint is continuously applied for protection. Simultaneously, therapeutic exercises focus on shoulder stretching, and range of motion exercises are customized for the wrist, hand, and fingers. However, it is crucial for patients to avoid any resistance exercises involving the elbow or wrist.
As the patient transitions into the second phase, which lasts from the end of the first week to four weeks after surgery, they begin full elbow flexion exercises. These are supplemented by a gradual increase towards full extension. The splint, which was previously essential, is now removed at the surgeon's discretion, usually during post-operative check-ups. At this point, no bracing is advised. Techniques such as applying heat before exercises and ice after exercises are also incorporated into the rehabilitation process. From weeks 4 to 6, patients are urged to achieve full elbow range of motion. If they have difficulty reaching full extension, passive counter-pressure techniques can be used to assist. No bracing is utilized during this phase. Additionally, emphasis is placed on wrist and forearm strengthening exercises, which are resistance-based. After the 6-week mark, rehabilitation is characterized by a return to full, pain-free elbow movement. Therapeutic exercises transition to more advanced strengthening routines. As patients regain strength and confidence, training specific to their sport is introduced. Activities such as throwing and hitting are gradually incorporated, in line with the individual's recovery rate. The ultimate goal is to ensure patients can safely and confidently resume their full range of activities as their post-operative condition allows.
Distal biceps tendon ruptures can result in diminished elbow flexion strength and forearm supination ability [37]. These ruptures, often caused by a strong eccentric contraction of the muscle [38], are relatively uncommon, with an annual incidence rate ranging from 1.2 to 9.6 per 100,000 individuals (Fig. 7) [39,40]. They are observed more frequently in middle-aged men [41]. Choosing not to undergo surgery can result in a decline in the power of both elbow and forearm movements [37]. Therefore, the preferred treatment for a ruptured distal biceps tendon is typically surgical repair. Post-operative procedures, including immobilization and the commencement of passive and active movements, are determined by the surgeon's specific guidelines. The primary goal of rehabilitation is to improve patient functionality and enable a successful return to their prior activities [42].
During the immediate postoperative period following biceps tendon repair, the focus of rehabilitation is on alleviating post-surgical pain and swelling, preserving the integrity of the surgical repair, and fostering optimal tissue healing. In the first week, patients are advised to avoid any elbow movement and to refrain from placing weight on the repaired limb. A posterior splint is used to provide necessary protection, particularly during this critical healing phase. By the second week, patients transition to progressive exercises, with an emphasis on controlled range of motion activities. These activities gradually shift from passive to more active movements. As patients move into the intermediate phase (2−6 weeks), they participate in targeted exercises designed to improve mobility. These exercises include shoulder and wrist activities, all while adhering to weight-bearing restrictions. The late postoperative phase, which spans from weeks 7 to 10, marks an advanced stage in the rehabilitation process. The objectives during this period are to consolidate the surgical repair and fine-tune scapulothoracic mechanics. Weight-bearing on the elbow is introduced in the eighth week and is progressively increased. Combined motion exercises become a crucial part of the regimen, with composite activities such as forearm planking and quadruped progressions being introduced. Efforts are also made to strengthen the scapulothoracic region, using exercises like wall slides and seated retractions [15,42].
Rehabilitation Strategies after Elbow Arthroscopy
Elbow arthroscopy offers several advantages when treating conditions such as lateral epicondylitis and elbow osteoarthritis. This procedure allows for direct visualization of intra-joint components through minimal incisions, thereby reducing scarring, inflammation, wound complications, and the risk of heterotopic ossification (HO). These advantages lead to less postoperative discomfort and expedite rehabilitation, facilitating a faster return to daily activities and sports [43]. A hallmark of the arthroscopic technique, particularly relevant to conditions like lateral epicondylitis, is the immediate commencement of rehabilitation, often on the day of surgery or the following day. This is subject to individual post-surgical responses, including factors such as anesthesia-induced nausea or personal pain thresholds. Patients can benefit from edema control techniques, which include rest, ice, compression, and elevation, or the use of compression garments and cold compresses [43]. Active range of motion exercises, crucial for managing conditions like elbow osteoarthritis, are initiated with the primary dressing still in place on the day of surgery. By the next day, this dressing can be removed, allowing for an increase in range of motion exercises based on the patient's comfort levels. In the case of lateral epicondylitis, post-debridement stretching exercises for the forearm muscles are implemented [44], and putty exercises are introduced early for minor grip strengthening and edema reduction [45]. This proactive approach contrasts with the more conservative postoperative care seen in open elbow procedures, where the arm might be immobilized for up to 2 weeks in a brace or post-surgery cast, usually maintaining the elbow in a 90° flexed position.
Postoperative Rehabilitation Strategies for Elbow Trauma Surgery
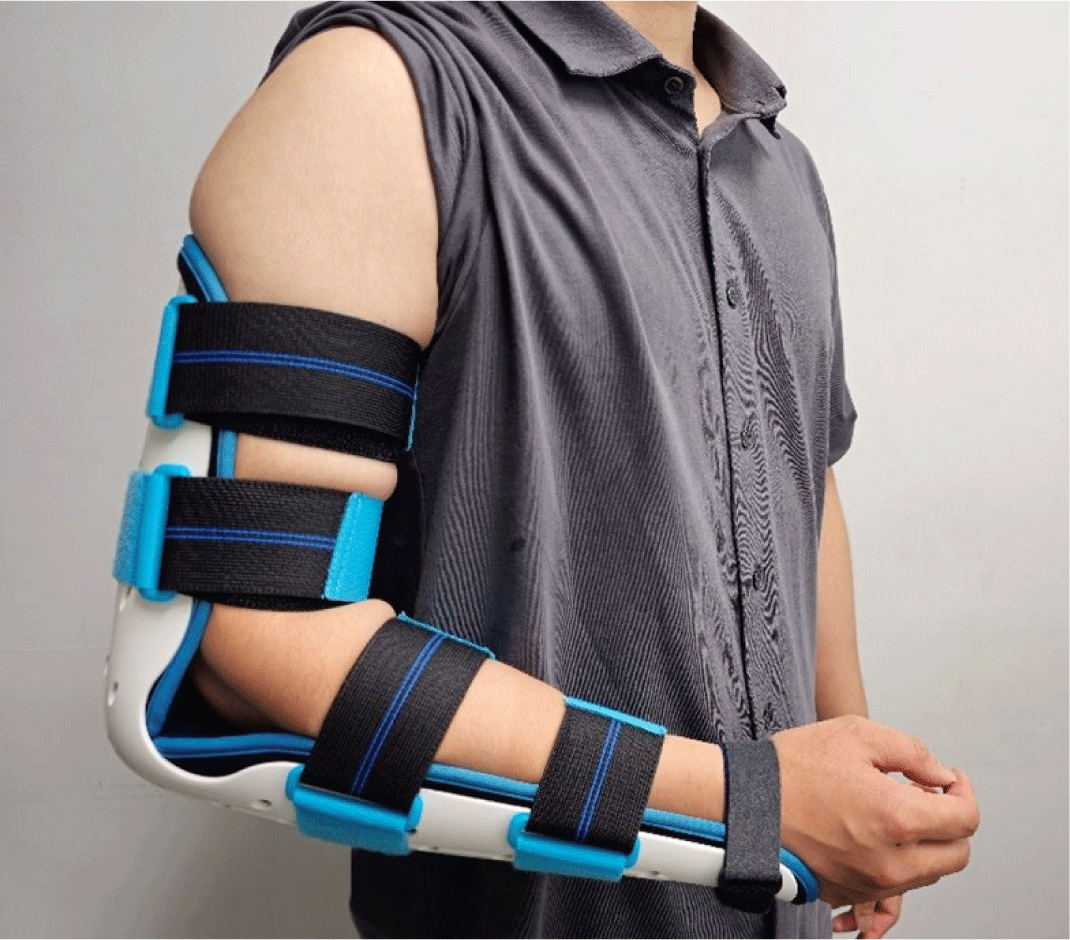
Trauma to the elbow joint can range from simple dislocations to more complex injuries such as fractures of the radial head/neck, proximal ulna (olecranon), distal humerus, and fracture dislocations like the terrible triad. Managing traumatic elbow injuries can be relatively challenging due to the joint's complex anatomy and the typically complicated nature of the injury, which can involve the bony structure, ligaments, nerves, and soft tissue. Common complications include post-traumatic stiffness, HO, arthritis, nerve injury, and soft tissue-related issues such as infection [46]. Therefore, while the postoperative rehabilitation program should be tailored to each patient, one of the key objectives in rehabilitating elbow trauma-related surgery is the prevention of stiffness [47]. Prolonged immobilization is a risk factor for developing stiffness, while early mobilization can facilitate quicker recovery and return to work without jeopardizing the stability of the fixation. However, since ligament injuries are common in traumatic elbow injuries, ligament repair or reconstruction is often necessary. To prevent re-rupture or instability of the repaired side, protection from varus/valgus stress should be provided through a hinged brace. This brace can control the angle of flexion/extension to avoid stressing the valgus/varus direction (Fig. 3). Additionally, HO can cause stiffness. To prevent the development of HO, the use of NSAIDs should be considered postoperatively.
Conclusion
The complex anatomy and functionality of the elbow make postoperative rehabilitation essential for optimal recovery. Tailored rehabilitation programs, designed according to the specific pathology or procedure, can lead to improved functional outcomes, fewer complications, and a faster return to daily activities following surgery. The fundamental principles of rehabilitation encompass accurate diagnosis, management of pain and swelling, early initiation of motion exercises, and the maintenance of neuromuscular stability. Adopting a patient-centric approach, which understands and caters to individual needs and preferences, and incorporates modern technology such as telehealth and YouTube for educational purposes, can further enhance postoperative care. Future research should aim to refine rehabilitation protocols in order to minimize complications and facilitate even quicker recovery trajectories.